The treatment of psoriasis should be based on shared decision between patients and their doctors. Patients should be given adequate information regarding their disease and current available treatment options. The goal of treatment is to improve and maintain patients’ quality of life through control of symptoms and signs of psoriasis. Implementing and regular monitoring of treatment goals based on disease severity and patients’ preferences are necessary to ensure long-term effective treatment and to prevent complications from uncontrolled disease activity. The choice of treatment should be individualized based on patient’s disease severity, patient’s preference, availability of treatment and the risk-benefit of treatment.
Modalities of Treatment for Different Types of Psoriasis
There are various treatment modalities available for psoriasis depending on the type of psoriasis, disease severity, patient’s preference, availability of treatment and the risk-benefit of treatment. Treatment options currently available include topical treatment, systemic treatment, phototherapy and biologics.
Topical therapy is generally indicated for mild to moderate disease. However, even patients with extensive psoriasis can be effectively treated with topical therapies provided patients are compliant to their treatment. Topical therapies that are currently available in Malaysia include moisturizers1 for skin dryness, tar-based preparations2 for the thick and scaly skin lesions, corticosteroids3 to reduce inflammation, vitamin D analogues4 such as calcipotriol to also reduce inflammation, calcineurin inhibitors5 such as tacrolimus for psoriasis affecting the face and skin folds, and salicylic acid6 to thin the thickened lesions (keratolytic) (Photo 1).
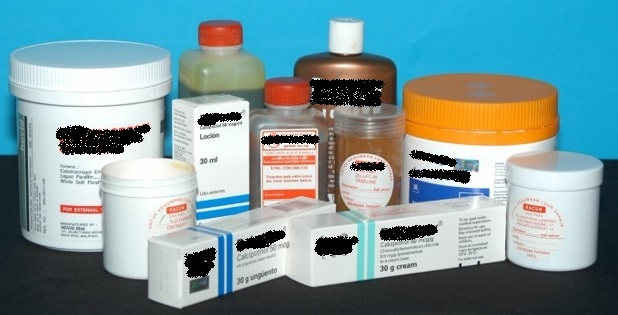 |
| Photo 1: Various topical treatment |
Phototherapy7,8 is indicated for patients with moderate to severe chronic plaque psoriasis. It includes ultraviolet A (UVA), ultraviolet B (UVB), red light, blue light and excimer laser. UVA is delivered in combination with a photosensitizing agent (psoralen) in oral, topical or bath form. UVB is delivered as narrowband (NBUVB) or broadband (BBUVB) (Photo 2). Patients need to undergo 2-3 sessions of phototherapy per week.
 |
| Photo 2: Phototherapy cabin |
Patients with moderate to severe psoriasis frequently require systemic or biologic therapy. Systemic agents such as methotrexate9, acitretin10 and cyclosporine11 have possible significant side-effects and cumulative toxicity. Therefore, pre-treatment assessment of patients is important to identify those at risk of developing toxicity. Laboratory/imaging tests should be done at baseline and at regular intervals to monitor for side effects/toxicity.
There are strong and consistent evidences on the efficacy of biologics in the treatment of moderate to severe plaque psoriasis12. Biologics such as infliximab, adalimumab, ustekinumab and etanercept are bioengineered proteins designed to block specific molecular steps important in the pathogenesis of psoriasis. However, biologics are associated with adverse events of which some are serious and life threatening. These include opportunistic infections, reactivation of tuberculosis, malignancy, congestive heart failure, demyelinating disease, injection/infusion reactions, hematological disturbances and liver toxicity. All current available biologics are administered with injections.
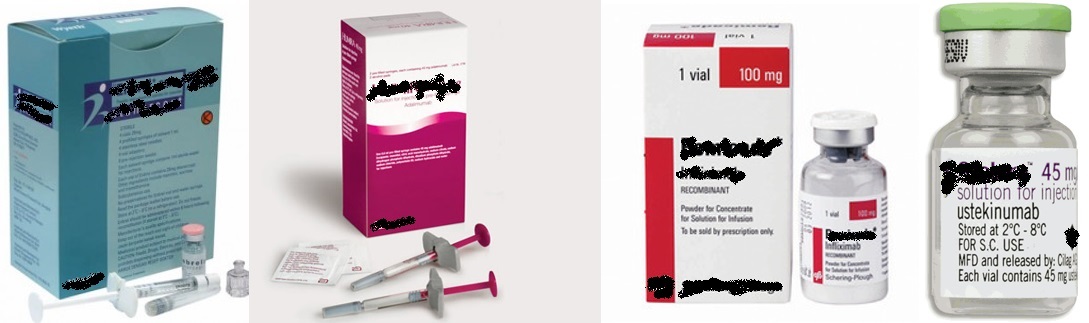 |
| Source: Open access, Google Images |
Treatment of psoriasis in pregnant patients that are considered relatively safe include moisturizers, topical corticosteroids, UVB phototherapy, oral cyclosporine and systemic corticosteroids.
How to Maximize Effects of Treatment
Patient adherence to the treatment regime prescribed by their doctor is the key component in ensuring they receive maximal effects of treatment. Implementing and regular monitoring of treatment goals based on disease severity as well as monitoring side effects and toxicity of treatment, are necessary to ensure long-term effective treatment and to prevent complications from uncontrolled disease activity.
Why is Systemic Steroids Discouraged?
The use of systemic steroids is discouraged because of several reasons:
- Patients on high-dose and/or prolonged use of systemic steroids are at risk of developing long-term side effects such as Cushing’s syndrome, diabetes, hypertension, osteoporosis, cataracts, peptic ulcers, acne and suppression of naturally-occurring hormones in the body.
- Patients on systemic steroids cannot be weaned of the steroids quickly, therefore increasing their risk of long-term steroid-related complications. If the systemic steroids are withdrawn abruptly, psoriasis lesions become unstable and may suddenly extend to involve the entire body (erythroderma), or develop into pus-filled blisters (generalized pustular psoriasis), both of which can be life-threatening.
Reference
- Watsky KL, Freije L, Leneveu MC. Water-in-oil emollients as steroid-sparing adjunctive therapy in the treatment of psoriasis. Cutis, 1992 50(5):383-386
- Slutsky JB, Clark RA, Remedios AA, et al. An evidence-based review of the efficacy of coal tar preparations in the treatment of psoriasis and atopic dermatitis. J Drugs Dermatol, 2010 9(10):1258-1264
- Mason AR, Mason J, Cork M, et al. Topical treatments for chronic plaque psoriasis. Cochrane Database Syst Rev, 2009 15(2):CD00502
- Kragballe K, Austad J, Barnes L, et al. A 52-week randomized safety study of a calcipotriol/betamethasone dipropionate two-compound product .(Dovobet/Daivobet/Taclonex) in the treatment of psoriasis vulgaris. Br J Dermatol, 2006. 154(6):1155-1160.
- Lebowhl M, Freeman AK, Chapman MS, et al. Tacrolimus ointment is effective for facial and intertriginous psoriasis. J Am Acad Dermatol, 2004. 51(5):723-730
- Carroll CL, Clarke J, Camacho F, et al. Topical tacrolimus ointment combined with 6% salicylic acid gel for plaque psoriasis treatment. Arch Dermatol, 2005. 141(1):43-46
- Medical Advisory Secretariat. Ultraviolet phototherapy management of moderate-to-severe plaque psoriasis: an evidence-based analysis. Ontario Health Technology Assessment Series, 2009. 9((27)
- Archier E, Devaux S, Castela E, et al. Efficacy of psoralen UV-A therapy vs. narrowband UV-B therapy in chronic plaque psoriasis: a systematic literature review. J Eur Acad Dermatol Venereol, 2012 (Suppl 3):11-21
- Saurat JH, Langley RG, Reich K, et al. Relationship between methotrexate dosing and clinical response in patients with moderate to severe psoriasis: subanalysis of the CHAMPION study. Br J Dermatol, 2011 165(2):399-406
- Bansback N, Sizto S, Sun H, et al. Efficacy of systemic treatment for moderate to severe psoriasis: Systematic Review and Meta-analysis. Dermatology 2009. 219:209-218.
- Heydendael VM, Spuls PI, Opmeer BC, et al. Methotrexate versus cyclosporine in moderate-to-severe chronic plaque psoriasis. N Engl J Med, 2003 349(7):658-665
- Reich K, Burden AD, Eaton JN, et al. Efficacy of biologics in the treatment of moderate to severe psoriasis: a network meta-analysis of randomized controlled trials. Br J Dermatol, 2012 166(1):179-188
| Last Reviewed | : | 23 August 2019 |
| Writer | : | Dr. Rajalingam a/l Ramalingam |
| Accreditor | : | Datin Dr. Asmah bt. Johar |
| Reviewer | : | Dr. Nazatul Shima bt. Abd Rahim |







