Systemic Lupus Erythematosus (SLE), or lupus, is an autoimmune disorder where the immune system produces antibodies that attack the body’s own tissues, causing inflammation in many different parts of the body such as the skin, joints, brain, lungs, heart and kidneys.
SLE predominantly affects women between 12 and 45 (the years they can bear children). Advances in treating SLE over the years has resulted in better care outcome in these women. As a result, pregnancies in this group of patients are increasingly common and generally successful. However, pregnancies in these women are still associated with higher rates of maternal and foetal. A death and illness successful pregnancy would require close monitoring and care involving specialists in different fields like obstetrics and rheumatology.
Is It Possible For Me To Get Pregnant If I Have SLE? (Ability to get pregnant)
Your fertility is usually not affected to a great degree by SLE, but you may face fertility issues if you have received certain drugs or have an associated condition called antiphospholipid syndrome. In these cases, you may have trouble conceiving or may experience pregnancy losses.
Pregnancy is not discouraged but it has to be planned with your rheumatologist and other specialist caregivers. You should always discuss your intention for a pregnancy with your doctors to ensure that you are in optimal health for the pregnancy. You should inform your doctor(s) as soon as you are aware you are pregnant: your doctor(s) may want to run additional tests and provide counselling. Your doctor(s) will do their best to support you through your pregnancy.
As with pregnancies in other women who do not have pre-existing medical conditions, you should be as fit as possible for the pregnancy. Therefore it would be advisable for you to stop smoking or taking alcohol before you conceive.
It is also advisable to consult your doctor about how stable your disease is and if you have any reasons it is unsafe to get pregnant. There is a small group of women for whom doctors would advise against pregnancy as the pregnancy would pose a significant risk to their health. These women are those with:
- pulmonary hypertension
- severe kidney disease
- severe lung disease
- recent severe active disease or flare
It would be highly advisable to wait for at least 6 months after a flare, or to have a period of little or no disease activity for at least 6 months before attempting conception.
Will My Disease Flare During Pregnancy?
Generally, if the disease is well-controlled at conception and you do not have severe kidney disease or pulmonary hypertension, you are unlikely to develop significant complications during pregnancy. You will be monitored very closely by your rheumatologist and obstetrician during your pregnancy. You will be scheduled for more frequent reviews in order to detect problems early. Therefore it is essential that you attend all your appointments.
There is a risk of a flare of your disease after delivery, but you will be monitored closely and should not stop your medications, unless advised by your rheumatologist. However, if you do get a flare, they are generally mild and easily managed with minor adjustments in the dosages of your medications.
In addition to your medical care, you are advised to adopt a healthy lifestyle throughout your pregnancy, i.e. you should eat a well-balanced diet and get adequate exercise, to ensure your pregnancy progresses optimally.
What Are The Potential Complications During Pregnancy?
Pregnant patients with SLE are at increased risk of pre-eclampsia, pre-term births, miscarriages and babies which do not grow optimally in the womb. Pre-eclampsia is a form of hypertension that occurs in pregnancy. The risk of pre-eclampsia is 1 in 5 lupus pregnancies.
There are two particular groups of antibodies which can cause problems during pregnancy: the antiphospholipid antibodies and the anti-Ro and anti-La antibodies.
A small percentage of women with SLE will have the antiphospholipid antibodies. These antibodies make the blood ‘sticky’. This combination increases the risk of blood clots, miscarriages, pre-eclampsia and your baby not growing optimally in the womb. You will need specific treatment with medications like aspirin and heparin to reduce the risk of the above complications. Many women who receive these treatments go on to have successful pregnancies.
Babies exposed to the anti-Ro and anti-La antibodies may be born with a condition called ‘neonatal lupus syndrome’. They may have a lupus-like rash and/or a slow heart rate.
The rash occurs in 10% (1 in 10 babies) of babies exposed to the antibodies (Figure 1). The rash can appear frightening but the baby is unaffected by it. It goes away completely by the time the baby is 6 months old and does not have any lasting effects on the baby. There is no evidence that the baby will develop SLE later in life.
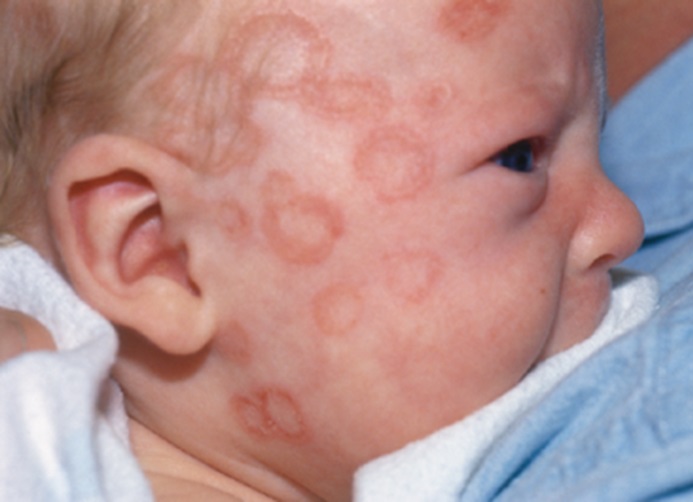 |
| Figure 1: rash of the neonatal lupus syndrome |
The slow heart rate is more dangerous because it can threaten the life of your baby, but it is much less common than the rash. The risk of the baby having a slow heart rate is about 2%, ie 1 in 50 babies. In majority of cases, this occurs between 18-24 weeks of pregnancy. What happens in these pregnancies is that the antibodies cross the placenta and stick to the ‘electrical circuits’ in the baby’s heart. You will be scheduled for regular monitoring and scans of the baby’s heart during your pregnancy.
Would I Need To Stop My Drugs During Pregnancy?
You should consult with your rheumatologist about the drugs you are taking because certain drugs can affect your ability to conceive, may have an effect on the development of your unborn baby and your health.
The following drugs should be avoided during pregnancy:
- Immunosuppressive agents: methotrexate, leflunomide, cyclophosphamide, mycophenolate mofetil, rituximab, belimumab
- Painkillers: celecoxib, etoricoxib, meloxicam, diclofenac, ibuprofen, indomethacin, naproxen
- Anticoagulants: warfarin, dabigatran
- Anti-hypertensives: perindopril, captopril, losartan, valsartan
- Antacids: omeprazole, pantoprazole, lansoprozole
- Antibiotics: ciprofloxacin, moxifloxacin
If you are on these drugs, you will be asked to stop them for a certain period of time before being allowed to get pregnant because these drugs have been associated with foetal malformations. However, if you do fall pregnant while taking these drugs, you have to inform your doctor as soon as possible. These drugs will be discontinued immediately and switched to alternative drugs, if needed, and the unborn baby will be monitored very closely by the obstetrician. There are certain painkillers which can be taken in early pregnancy, if necessary, but you should discuss this with your doctor.
The following drugs can be safely taken during pregnancy:
- Immunosuppressive agents: azathioprine, ciclosporin, prednisolone
- Anti-malarial: hydroxychloroquine
- Painkillers: paracetamol, tramadol
- Anticoagulants: heparin
- Anti-hypertensives: nifedipine, methyldopa, labetolol
- Antacids: ranitidine
- Antiplatelet agents: aspirin
- Calcium and vitamin D
- Folic acid
Drugs like hydroxychloroquine and prednisolone, which are the mainstay of therapy, are safe in pregnancy and lactation. Most women tolerate these drugs well during pregnancy. You will be advised not to stop taking them to ensure a successful pregnancy.
It is very important you do not stop prednisolone during pregnancy unless instructed by your doctor because it may cause your disease to flare. Your doctor will try to keep your prednisolone dose as low as possible, i.e. less than 10mg per day.
Hydroxychloroquine has been shown in many studies to be beneficial in keeping your disease under control and also in reducing the risk of slow heart rate in the babies of mothers who have the anti-Ro/La antibodies.
Many antibiotics are also safe to be taken during pregnancy. Please check with your doctor before taking any unknown medications.
Can I Deliver Normally?
There is no reason why you cannot deliver normally. However, as the antenatal care of women with lupus is often individualised, some women may require a Caesarean section if problems arise. Your obstetrician will discuss delivery plans with you closer to your due date.
It would be best to deliver in the hospital where you had your specialist antenatal care. However, if this is not feasible, it would be highly advisable to deliver in a hospital which provides good neonatal care.
Should I Test My Baby For Lupus?
Less than 10% of children born to women with SLE will develop SLE later in life. There is presently no test to reliably predict if your baby will develop SLE later. As the baby has received a mixture of genes from you and your partner, it is possible that the baby would not have inherited enough genes to cause lupus. Even if your baby had inherited the genes, there are still unknown external factors that need to be involved in order for your baby to develop lupus.
Can I Breastfeed My Baby?
Yes, you can. The drugs which you have been taking during pregnancy can also be used safely while breastfeeding.
Conclusion
Many women with SLE go on to have successful and enjoyable pregnancies, resulting in healthy babies. It is most important that every pregnancy is planned: the rheumatologist has to assess your disease activity, drugs, anti-Ro/La antibody status, antiphospholipid antibody status before allowing you to go ahead with conception.
References
Lateef A, Petri M. Management of pregnancy in systemic lupus erythematosus. Nat Rev Rheumatol. 2012 Dec;8(12):710-8. doi: 10.1038/nrrheum.2012.133. Epub 2012 Aug 21.
| Last Reviewed | : | 16 October 2017 |
| Writer | : | Dr. Ding Hui Jen |
| Accreditor | : | Dr. Mollyza bt. Mohd Zain |







