When is a baby considered preterm?
Most babies are born at around 40 weeks of gestation. Babies are considered term if born between 37 and 42 weeks. If born before 37 weeks they are considered preterm.
Are many babies born preterm?
Incidence of prematurity varies in different countries. About 8% of babies are born preterm in Malaysia.
Why are babies born preterm?
Causes are often unknown, but are sometimes associated with :
- Premature rupture of membrane which may be triggered by infections of amniotic fluid and fetal membranes
- Preterm labour
- Previous preterm birth
- Multiple pregnancies eg twins and triplets and even higher order
- Uterine or cervical abnormalities
- Pregnancy related complications e.g. pregnancy induced hypertension and placenta praevia
- Poor social support
- Maternal consumption of alcohol, illicit drugs or smoking
- Urinary tract infections
- Congenital intrauterine infections
- Congenital abnormalities
How does a preterm baby look and behave?
- A preterm baby is borns small in size and has immature features, severity of which depends on the degree of prematurity.
- Birthweight for preterm babies usually ranges from 500 gm for a 22 weeks gestation to 1000 gm for a 28 weeks and 1500 gm for 32 weeks and 2.5 kg for 37 weeks baby.
- Signs and symptoms vary according to the presence of complications.
- May have signs of respiratory distress (such as grunting, flaring of nose, chest recessions, increased rate of breathing and a bluish hue to the skin) and temperature instabilty.
Should we be worried if babies are born preterm?
Prematurity is associated with many potential complications, the more preterm, the higher risk for each complication. Early and late complications include:
- Respiratory distress syndrome (RDS) due to deficiency of a substance called surfactant in the lungs.
- Intraventricular haemorrhage (IVH) i.e. bleeding involving fragile capillaries around the ventricles in the brain.
- Jaundice (yellowish discolouration of skin and sclera) due to immature system of bilirubin metabolism.
- Feeding difficulty/intolerance due to immature gut.
- Infections involving blood (septicaemia), lungs (pneumonia), membranes surrounding brain and spinal cord (meningitis) and intestines (necrotising enterocolitis / NEC) .
- Retinopathy of prematurity (ROP), a condition of abnormal growth of blood vessels in the eye.
- Chronic lung disease resulting from lung damage due to prematurity, and oxygen and ventilation therapy.
- Connecting vessel between the heart and the lungs), remaining patent (Patent Ductus Arteriosus) which may result in breathing difficulties or heart failure.
- Inguinal hernia which is due to weakness of the muscles in the groin area.
Late complications include :
- Cerebral palsy
- Mental retardation
- Epilepsy
- Blindness
- Deafness
- Learning disability
- Delayed development
- Poor growth such as short stature
Mortality rate is high even with intensive care, babies born between 26 and 28 weeks gestation have a mortality rate of 30-50% while babies born before 26 weeks have a mortality of between 80 to 100%.
More mature preterm babies have good survival rate of up to more than 90% in babies above 34 weeks.
Do preterm babies need any special treatment?
The care needed will depend on the severity of the prematurity and the condition of each baby. General care needed for all preterm babies :
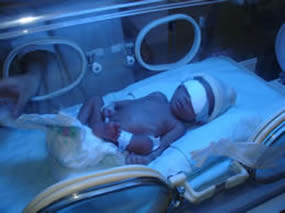
- Temperature control
- May need nursing in incubator or under radiant warmer (as shown in picture below).
- Blood sugar monitoring
- To detect and treat high or low blood sugar levels.
- Provision of Nutrition
- Borderline preterm babies above 35 weeks who are otherwise well can usually be breastfeed exclusively. More preterm babies often need supplementation with formula milk in the early days. Expressed breast milk is important to enhance gut maturity as well as to reduce the risk of infection.
- Prevention of infection
- Hand washing is of prime importance before and after handling preterm babies.
Specific treatment depends on the condition of the child and existing complications e.g. :
- Ventilation and surfactant therapy for RDS
- Close monitoring of oxygen therapy
- Fluid and electrolyte management in sick babies
- Parenteral nutrition (i.e. nutrition given directly into the veins) in babies who are not able to take milk through the gastrointestinal tract. Expressed breastmilk or formula milk is usually fed via an oro-gastric tube in very preterm babies who are able to tolerate enteral feeding
- Antibiotics when infection is suspected or confirmed
- Ultrasound scanning of the brain for detection and management of IVH and other abnormalities
- Screening for ROP and laser or cryotherapy treatment for those who have serious eye disease
- Home oxygen for those with chronic lung disease who is otherwise able to be nursed at home
Ethical Issues
- Counselling and support to parents are given to help them understand their baby’s condition and to reach realistic expectations
- Withholding intensive care should be considered for the very extreme preterm baby such as below 25 weeks gestational age or below 500 grams birthweight as these babies are unlikely to survive. For those of 25 weeks gestation, of the 20% of babies who survive, 80 % will have poor neurological outcome
- Withdrawal of intensive care and palliative care should be given to babies who are unlikely to survive in the long term or where the quality of life is very poor. These include babies who have had multiple complications such as respiratory failure, severe NEC or severe IVH
Can anything be done to prevent preterm births?
Prevention of preterm births
- Women to avoid smoking, illicit drugs and alcohol
- Prepregnancy care for women with chronic medical conditions eg diabetes
- Minimise embryo transfer to reduce multiple pregnancy in assisted reproductive technique
- Early and regular antenatal care to identify and treat problems promptly
Reducing risk of complications of prematurity
- Mother to see doctor promptly when there is any contraction of the uterus, leaking of liquor, fever
- Use of antenatal corticosteroid when a preterm delivery is suspected, speeds maturation of the lungs and reduce risks of RDS, IVH, NEC and infant death
- Use of tocolytic may postpone labour and delay delivery for a few days to allow steroid time to act.
- Antibiotics for mothers who have “burst water bag” i.e. rupture of membranes and in preterm labour
- Transfer of mother in preterm labour to deliver in a hospital with a neonatal intensive care unit
Rehabilitation is an important aspect of management
On discharge:
- Need to continue with whatever medications that have been prescribed including vitamin and iron preparation.
- Nutritional needs of baby. Patience is required when feeding very preterm babies as they are usually very slow feeders. Breastfeeding is ideal but when formula milk feeding is used most will require a post-discharge formula milk for preterm babies to ensure increased protein and caloric and mineral contents so as to meet the higher needs of preterm babies.
- Following routine schedule for childhood immunisation
- Come for all follow up appointments given before discharge.
- Avoidance of overcrowding to prevent child from getting infections like chest infections
- Placing baby to sleep in the supine position
Follow-up of very preterm babies (< 32 weeks) is important to :
- Assess growth and development and to manage complications
- Assess for any hearing impairment as preterm babies who have been ill are at risk of hearing loss
- Assess for visual impairment as the preterm baby is at risk of myopia and to follow up for the resolution of any ROP
Some children will need :
- Physiotherapy and occupational therapy and other therapies
- Hearing aids
- Visual aids or operation
- Special education
| Last reviewed | : | 28 August 2020 |
| Writer | : | Dato’ Dr. Lim Nyok Ling |
| Dr. Lim Sern Chin | ||
| Reviewer | : | Dr. Zainab bt. Kusiar |







