Periodontal abscesses result from rapidly-growing bacteria within a periodontal pocket.
A periodontal pocket forms in the presence of periodontal disease, as the gums become infected and pull away from the surface of the teeth. This deepens the sulcus (the space between the teeth and gums) greater than three millimetres. The deepened sulcus is called a periodontal pocket.
What causes this condition?
An abscess forms when the pocket deepens to the point that plaque bacteria, calculus and/or food become trapped within it, and the body’s immune system cannot adequately combat the infection. A large swelling develops on the gums as a result of this uncontrolled, rapid growth of bacteria, bacterial products and infected gum tissue. As a result, what occurs is a fast, painful destruction of the supporting connective tissue and bone that surround the tooth.
Periodontal abscesses form anywhere along the side of the gums where the periodontal sulcus has deepened to become a pocket. They are common in cases of advanced periodontal disease, when bone loss has occurred as a result of the infection, because the pocket depth of five millimetres or more creates an ideal environment for abscess formation.
What symptoms may occur?
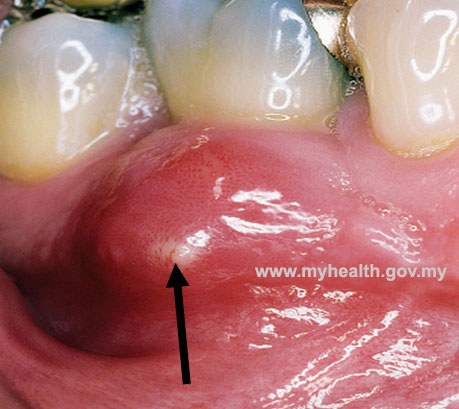
The most common of the periodontal abscess symptoms is a swelling in the gum. Any swelling can vary greatly in size, and may arise quite quickly. It will have a red, often shiny appearance and may have a white ‘head’. This swelling will be very tender to touch. Pain, which may be severe, usually accompanies an acute flare-up.
Other symptoms that may occur include:
- Bad breath
- Bleeding from the area
- The affected tooth or teeth may become noticeably looser and may drift slightly, leading to spacing between the teeth.
Clinical features of periodontal abscess
- Presence of generalized periodontal disease with pocketing and bone loss.
- Tooth is usually vital
- Loose teeth
- Overlying gingival erythematous, tender and swollen.
- Mild discomfort to severe pain
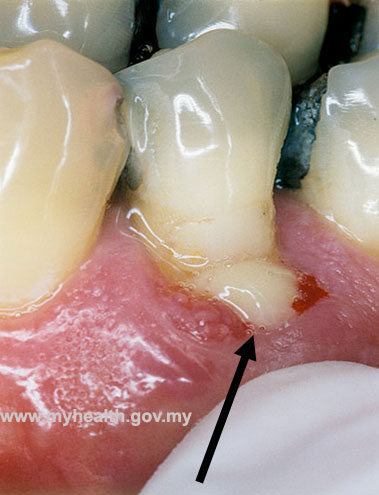
- Pus discharge via periodontal pocket or sinus opening
The causes of periodontal disease (which can lead to abscesses) include:
- Poor oral hygiene
- Smoking cigarettes
- Some medical conditions such as uncontrolled diabetes
People with reduced immune function, due to some diseases like diabetes or side effect of medical treatment for example corticosteroid or chemotherapy is at an increased risk of abscesses in general.
There are three types of abscesses associated with the periodontal tissues:
- Gingival abscesses
- Periodontal abscesses
- Pericoronal abscesses
Gingival abscess
A localized, purulent infection involves only the soft gum tissue near the marginal gingiva or the interdental papilla.
Periodontal abscess
A localized, purulent infection involves a greater dimension of the gum tissue, extending apically and adjacent to a periodontal pocket. Such a lesion may contribute to destruction of the periodontal ligament and alveolar bone.
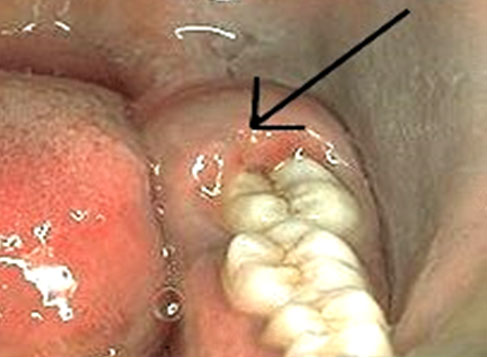
Pericoronal abscess
A localized, purulent infection exists within the gum tissue surrounding the crown of a partially or fully erupted tooth. This is also referred to as pericoronitis
Periodontal abscess treatment
If you have any of the above symptoms, particularly if a swelling is spreading quickly (cellulitis), then seeks immediate advice from your dentist. Any treatment will vary depending on how severe the dental abscess is.
Here are the general steps taken:
- Drainage of the pus, via the gum (usually) or an incision in the swelling
- Antibiotics may be needed if it involved patient systemic condition
- Scaling of the area to clear any tartar and plaque and help the gum heal
- Periodontal surgery may be needed in certain condition
- Root canal may be needed in the case of a ‘perio-endo’ lesion. Here both the pulp and periodontal tissues are infected. Where extraction of the affected tooth is the only option this will be carried out.
It is best to get treatment early, not only for health reasons (as abscesses can be dangerous), but also for a better prognosis. A periodontal abscess can quickly destroy the gum tissues that hold a tooth in place. If left to fester, then the outlook for the tooth can be very poor.
| Last Reviewed | : | 3 October 2014 |
| Writer / Translator | : | Dr. Noordin b. Kasan |
| Accreditor | : | Dr. Uma Subramaniam |