Introduction
Osteoarthritis is a disease affecting the cartilage of a joint that is caused by injury or wear and tear of the joints over the years. It is the most common type of arthritis.
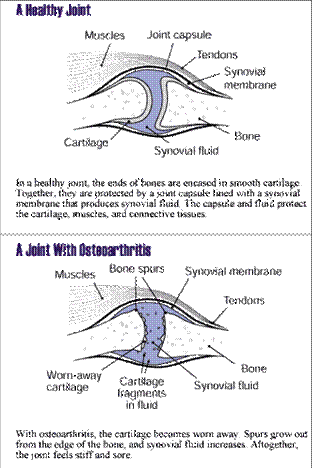
Cartilage is the slippery tissue that covers the ends of bones in a joint. Healthy cartilage allows bones to glide over one another. It also absorbs energy from the shock of physical movement.
Who gets osteoarthritis?
Can be divided into two common groups :
- Older age group – usually due to the process of wear and tear. This is more common.
- Younger age group – usually due to injury.
What causes osteoarthritis?
Osteoarthritis is an inevitable part of aging. Obesity, work related injuries and injuries due to sports are also part of the causes of osteoarthritis.
Individuals born with abnormal cartilage or with slight defects in the way that joints fit together may develop osteoarthritis. It can be divided into mild moderate and severe.
In osteoarthritis, the surface layer of cartilage breaks down and wears away. This allows bones under the cartilage to rub together, causing pain, swelling and loss of motion of the joint.
Over time, the joint may lose its normal shape. Also, bone spurs (small growths called osteophytes) may grow on the edges of the joint. Bits of bone or cartilage can break off and float inside the joint space. This causes more pain and damage.
How do you know you have this condition?
People with OA usually complain of joint pain associated with stiffness and reduced range of movement. Commonly, they have pain which worsens with activities.
Sometimes you can develop deformities of the affected joints.
How is it diagnosed?
Signs and symptoms as above and an x-ray can usually confirm the diagnosis. The common joints affected are as depicted below :

How is it treated?
The treatment depends on how the condition affects the patient. Basically the treatments are given to delay surgery if it is eventually needed.
- Medications (pain-killers or NSAIDs)
- Exercise/physiotherapy – muscle strengthening
- Activity modifications – reduction in strenuous activities/exercises
- Weight loss if obese or overweight
If the patient does not improve with the above measures :
- An intra-articular injection using synthetic material can be done, but this has a temporary effect and may need to be done repetitively (ie yearly).
Finally, if all of the above methods are not effective in relieving the pain, surgery (total joint replacement) is the final step.
If the patient can still live with the pain, surgery can be delayed until the patient gives up.
What are the complications of surgery?
Complications can be divided into early and late. Early complications include :
- Infection
- Deep vein thrombosis (blood clot in the calf vessel)
- Wound breakdown
- Complications related with the surgery ie blood loss and anaesthesia (adverse drug reaction)
Late complications include :
- Infection
- Loosening of the implants
- Fractures
- Failure of the materials used ie polyethylene
- Revision
References
Campbell Operative Orthopaedics
| Last reviewed | : | 25 April 2012 |
| Writer | : | Dr. Izan Ibrahim |
| Reviewer | : | Dr. Heselynn Hussein |







