What is HIV?
‘HIV’ stands for Human Immunodeficiency Virus, is the virus that attacks the immune systems, the body’s natural defense system. HIV attacks and destroys a type of white cell called a CD4 cell or T-cell. This cell’s main function is to fight diseases. When a person’s CD4 cell count gets low, they are more susceptible to illnesses. Over time, HIV can destroy so many of your CD4 cells and lead to AIDS, the final stage of HIV infection.
What is AIDS?
‘AIDS’ stands for Acquired Immunedeficiency Syndrome, is the syndrome which appears in advance stage of HIV infection. This is the stage of infection that occurs when the immune system is badly damaged and the person become vulnerable to opportunistic infection and illness; those illness said to be AIDS defining condition. When the number of CD4 cells falls below 200 cells percubic millimeter of blood (200 cells/mm3) , or develop one or more opportunistic illnesses (AIDS defining condition), the person is considered to have progressed to AIDS.
(AIDS defining illness e.g pneumocystis pneumonia, candidiasis, disseminated cytomegalovirus infection, severe herpes simplex virus infection, atypical mycobacterial infection, disseminated histoplasmosis, cryptococcal meningitis, lymphoma, toxoplasmosis of brain, kaposis sarcoma)
How do people get HIV?
Common ways people get HIV
- Share needles to inject drugs or steroid from an infected person. The diseases can also be transmitted by dirty needles used to make a tattoo or in body piercing.
- Have unproctected sex with an infected person.
- Receive a blood transfusion from the infected person.
- Born to a mother with HIV infection. A baby can also get HIV from the breast milk of an infected woman.
What are the signs of HIV/AIDS (oral manifestation) in the mouth?
Oral manifestation of HIV disease are common and include oral lesions and novel presentations of previously known opportunistic diseases. Studies have shown that 70%-80% of HIV infected individuals will develop at least one oral manifestation during the course of the disease. The presence of these lesions may be an indicator of HIV infection and predictor of the progression of HIV diseases.It should be stressed that the oral lesions in HIV infection are indicators and not truly specific for HIV diseases as several of them can also be found in non- HIV infected patient. The oral lesions in HIV patient are mainly infection (fungal, viral, bacterial), neoplasm, lymphadenopathy, immune-mediated, and other (xerostomia, pain syndromes, and nutritional).
A list of oral manifestations of AIDS is presented in Table 1
|
|
More common |
Less common |
| Infections Fungal |
Candidiasis | Aspergillosis Histoplasmosis Cryptococcosis Geotrichosis |
| Bacterial | HIV-associated periodontitis Necrotizing ulcerative gingivitis |
Mycobacterium avium Klebsiella pneumonia Enterobacter cloacae Escherichia coli Cat-stratch disease Sinusitis |
|
Viral
|
Herpes simplex virus (HSV) |
Human papillomavirus (HPV) |
|
Neoplasms |
Kaposi’s sarcoma |
Non-Hodgkin’s lymphoma |
|
Lymphadenopathy |
Cervical |
|
|
Neurologic |
|
Trigeminal neuralgia |
|
Miscellaneous |
|
Aphthous ulcerations |
Table 1 : A list of oral manifestations of AIDS
Fungal infection
Candidiasis
Oral candidiasis is the most common intraoral manifestation of HIV infection, predominantly due to Candida albicans. A healthy immune system can suppress the overgrowth of this fungus, but even a mildly weakened one may not keep it in check. Most outbreaks occur when CD4 count fall below 400 cell/mm3. Oral candidiasis has been reported to occur in 17–43% of patients with HIV infection and in more than 90% of patients with AIDS. The three common presentations of oral candidiasis are pseudomembranous candidiasis, erythematous candidiasis and angular cheilitis.
- Pseudomembranous candidiasis or thrush appears as multiple creamy white patches/plaques that can be rubbed off leaving red or bleeding underlying surface. This type most often affects the tongue, although every area of the oral mucosa may be affected. (Picture 1)
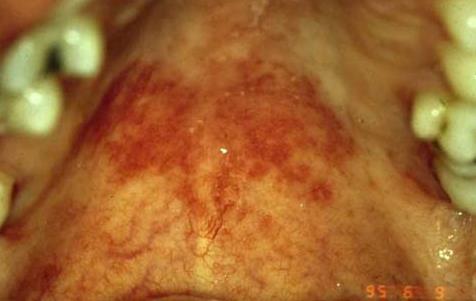
- Erythematous candidiasis appears as flat, red patches of varying size. It commonly occurs on the hard or soft palate. It may present as a “kissing” lesion- if a lesion is present on the tongue, the palate should be examined for a matching lesion, and vice versa. (Picture 2)
- Angular cheilitis
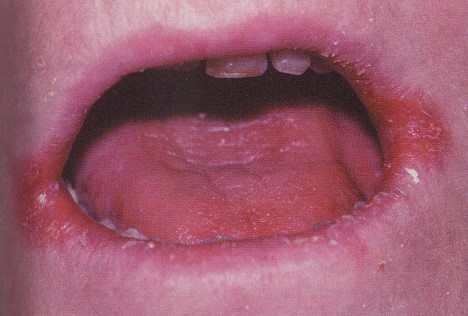
Angular cheilitis presents as erythema or fissuring either unilateral or bilaterally at the corners of the mouth. It can appear alone or in conjunction with another form of candidiasis. (Picture 3)
Treatment : The treatment of oral candidiasis includes topical and systemic antifungal medication. Topical therapy with nystatin and clotrimazole is effective for mild to moderate cases of oral candidiasis in individual with CD4 counts above 200 cell/mm3, however systemic antifungal therapy is frequently required in refractory cases and for severely immunocompromised patients.
Bacteria Infections
HIV associated periodontal diseases
Periodontal (gum) disease is common among HIV- infected patients. It is characterized by bleeding gums, bad breath, pain/discomfort, mobile teeth, and sometimes sores . HIV related periodontal diseases of bacteria origin can be classified into 3 forms
- Linear gingival erythema
Present as a 1-3 mm red band along the gingiva margin and may or may not accompanied by occasional bleeding and discomfort. It is seen most frequently in association with anterior teeth, but commonly extends to the posterior teeth. (Picture 4)
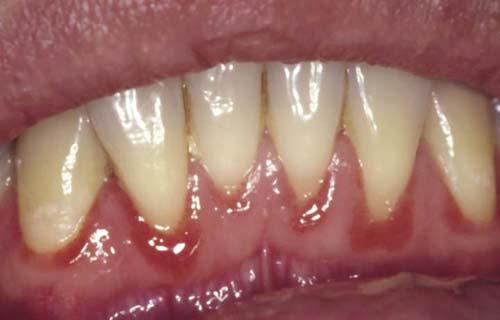
Picture 4- Linear gingiva erythema
- Necrotizing ulcerative gingivitis (NUG)
NUG is more common in adults than in chidren. It is characterized by the presence of ulceration, sloughing and necrosis of one or more interdental papillae with no loss of periodontal attachment and accompanied by pain, bleeding and fetid halitosis.
- Necrotizing ulcerative periodontitis (NUP)
NUP is a condition that causes pain,spontaneous bleeding of the gums and rapid destruction of gum tissue and bone, which may lead to tooth loss. Severe pain and spontaneous bleeding are common. (Picture 5)
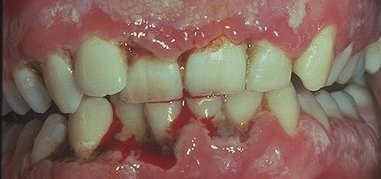
Picture 5- Necrotizing ulcerative periodontitisTreatment : The treatment of NUG and NUP consists of debridement of necrotic tissue and antimicrobial therapy. The administration of systemic antifungal medications and systemic antibiotic such as metronidazole, is of great benefit. Maintenance of good daily oral hygiene with brushing, flossing and use of mouthwash are effective ways to prevent and control periodontal diseases.
Viral infections
Herpesvirus accounts for the majority of HIV-related oral viral infections. Herpes simplex infection occurs as an intraoral and perioral variant. Most oral herpes simplex manifestation in HIV – infected patients are caused by herpes simplex type 1. The prevalence of oral HSV infection varies between 10% and 35% in HIV infected person. Recurrent intraoral herpes simplex and herpes labialis are seen in patients with HIV infection. The presence of HSV infection for more than 1 month constitutes an AIDS-defining condition.
Herpes simplex virus (HSV)
HSV infection appears as a crop of vesicles usually on the hard palate and gingiva and/or lips. The vesicles rupture and form irregular painful ulcers. HSV-1 can appear inside the mouth, often in palate. Sores usually occur with fever, pain and loss of appetite. Long standing herpetic infections in the oral cavity persisting for more than 3 weeks are associated with CD4 cell counts below 100 cells/mm3. Recurrent infections are generally more widespread, prolonged and chronic. (Picture 6)
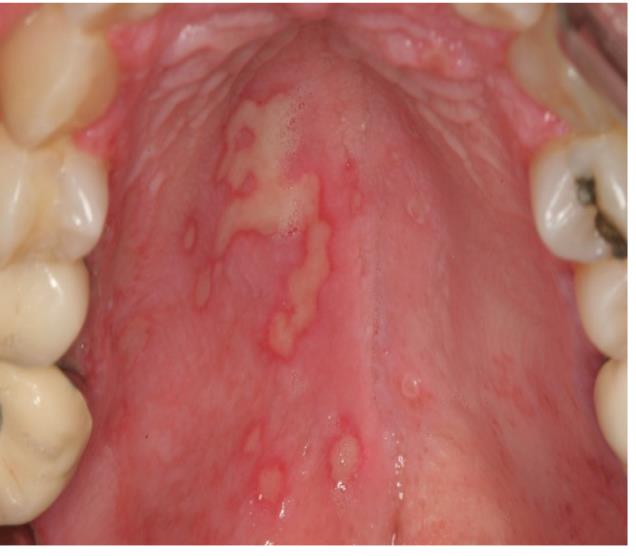
Picture 6- Herpes simplex infection.
Herpes labialis (also called cold sores)
Recurrent herpes labialis occurs on or around the lips. The patient may report a history of itching or pain, followed by appearance of small vesicles. These vesicles rupture and form crusted lesions. (Picture 7)

Picture 7- Herpes labialis
Treatment : Treatment for HSV infection includes systemic therapy with antiviral agents such as acyclovir or famciclovir. The treatment is more effective if it is instituted in the prodromal stage of infection. Foscarnet can be used for resistant infections.
Herpes zoster/Shingle
Varicella zoster virus (VZV) is a reactivation of the same virus that causes chicken pox. Recurrent VZV infection is fairly common in HIV infected patients, but the course is more severe. There are reports of increased incidence of Herpes zoster infection among HIV-infected patients. This occurrence can be severe, especially for those individuals with CD4 counts below 200 cell/mm3. Oral lesions begin as vesicles or ‘bubbles’ but they later burst to form ulcers or open sores, most commonly on the palate, distributed along a unilateral division of fifth cranial nerve. Patients often complain about severe pain. In HIV infected patients, the oral lesions are more widespread, chronic and result in a greater number of complication. (Picture 8)
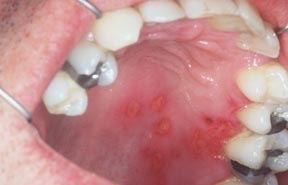
(Picture 8 – Herpes zoster)
Treatment : Generally, the treatment consists of high dose of acyclovir or valacyclovir or famciclovir.
Oral Hairy leukoplakia (OHL)
The most common EBV-related lesion in patients with AIDS is oral hairy leukoplakia. Oral hairy leukoplakia is a reliable indicator for HIV infection and a predictor for subsequent development of AIDs. The prevalence of hairy leukoplakia in HIV-infected patients varies from 20% to 36% or more and it is rare in children.
Oral hairy leukoplakia usually presents as a white, corrugated or folded lesion on the lateral borders of the tongue. The patches look like trush but can’t easily be removed. The lesions usually start on the lateral margins of the tongue and sometimes inside the cheeks and lower lip. They may be unilateral or bilateral, and they are painless. (Picture 9)
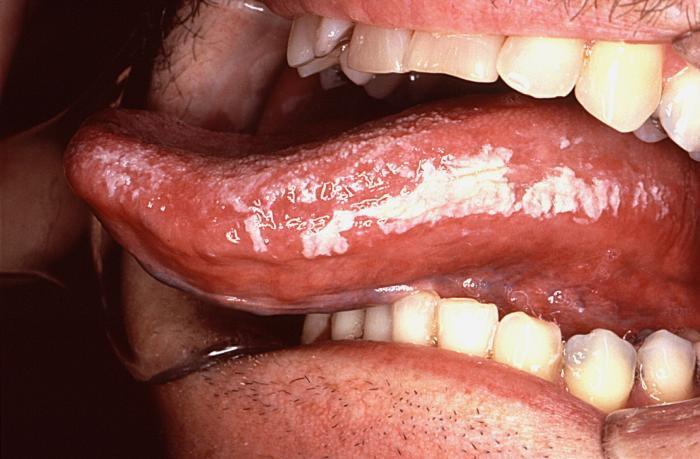
Picture 9 – Oral Hairy leukoplakia
Treatment : OHL usually does not require any treatment, but in severe cases systemic antivirals are recommended. The lesion usually regresses after oral administration of antiviral such as acyclovir for 1 or 2 months.
Human Papillomavirus (HPV) infection
An increased prevalence of HPV-infected lesions is noted in HIV-infected patients, and most are located in the anogenital areas. Oral involvement also may be seen. HIV lesions in the oral cavity may appear as solitary or multiple nodule with cauliflower-like growths, spikelike projections or slightly elevated sessile papules. They are painless. The most common location is the labial and buccal mucosa (cheek). (Picture 10)
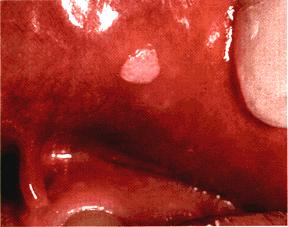
Picture 10- Human Papillomavirus infection
Treatment: Treatments for HPV include surgical removal, laser ablation, cryotherapy and topical application of keratinolytic agents.
Cytomegalovirus (CMV) infection
Oral manifestation of CMV is usually early sign of disseminated CMV infection. Oral CMV infection is associated with severe immune suppression. Oral manifestation of cytomegalovirus (CMV) is observed only in the patient with CD4 count below 100 cells/mm3 in the disseminated form of the disease. Mucosal CMV infections most frequently present as painful, large, sharply demarcated, and nonspecific ulcerations in any area of the oral mucosa.
Treatment : Intravenous (IV) ganciclovir or acyclovir may be given in high doses.
Neoplastic lesions
Kaposi’s sarcoma (KS)
Kaposis’s sarcoma is the most common AIDS-related cancer. The incidence of KS is much higher in homosexual men than other risk groups. It can be macular (flat), nodular or raised and ulcerated, with color ranging from red to purple; early lesions tend to be flat, red and asymptomatic with the color becoming darker as the lesion ages. The palate is the most common site, but they also occur on the gingiva and tongue. Oral kaposis sarcoma usually is not painful, but the lesions may interfere with chewing or talking. (Picture 11)
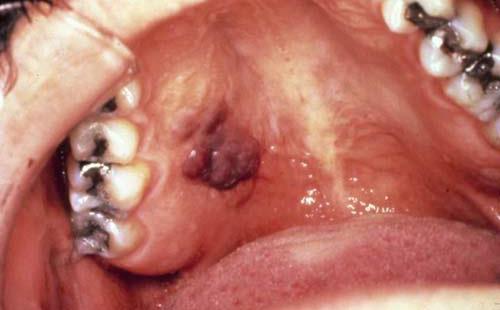
Picture 11- Kaposi’s sarcoma
Treatment : Management of oral Kaposi’s sarcoma includes local and systemic treatment depending on the clinical stage. The local treatment can be surgical or laser excision and radiotherapy. Systemic treatment is single or combined chemotherapy.
Non Hodgkin’s lymphoma( NHL)
Non-Hodgkin’s lymphoma is the second most common malignancy in HIV infection. The incidence of oral lymphoma in AIDS patients has increased in recent years. Unlike KS, NHL is more commonly detected in HIV – positive heterosexuals and injecting drug users. Oral NHL may be the first indication of either HIV infection or progression to AIDS.
Oral lymphoma commonly appears as a rapidly enlarging soft tissue mass, often with ulceration. Like KS, oral lymphoma is most frequently found on the palate and gingiva. The prognosis of patient with lymphoma remains poor, with survival rates of less than 25%. (Picture 12)
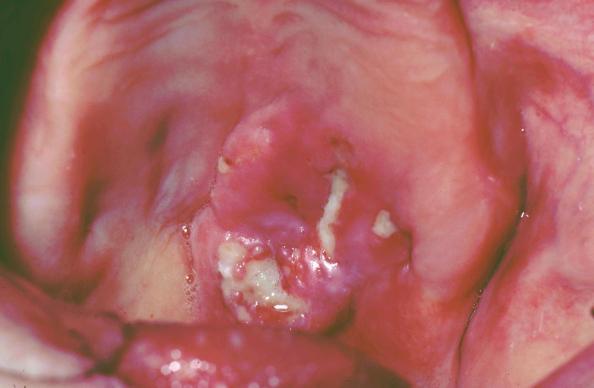
Picture 12 – Non Hodgkin’s lymphoma
Treatment: Treatment of oral lymphoma include multichemotherapy and radiation.
Persistent generalized lymphadenopathy (PGL)
PGL consists of lymphadenopathy that has been present for longer than 3 months. The most frequently involved sites are the posterior and anterior cervical, submandibular, occipital and axillary nodes. Nodal enlargement fluctuates, usually is larger than 1 cm and varies from 0.5 to 5.0 cm.
PGL does warn of progression to AIDS, almost one third of affected and untreated patients will have diagnostic features of AIDS within 5 years.
Treatment : Lymph node biopsy may be indicated in order to rule out lymphoma.
Miscellaneous HIV-related diseases
Recurrent Aphthous Ulcers
RAU is the most common immune-mediated HIV-related oral disorder occur in about 1%-7% of HIV-infected patients. They are painful ulcers commonly on the cheek (buccal mucosa), soft palate and tongue.The lesions are characterized by a halo of inflammation and a yellow-gray pseudomembranous covering. HIV positive patients tend to have more frequent, profound, and prolonged episodes of recurrent aphthous ulcers. Like other oral manifestations, these ulcerations are another marker for HIV progression and advanced immunosuppresion. Frequently, the ulcers are greater than 1 cm in diameter, extend deep into the submucosa, and respond poorly to topical medication. (Picture 13).
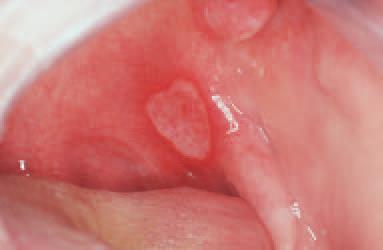
Picture 13 – Recurrent aphthous ulcer
Treatment : The first line of management of RAUs is pain control and prevention of superinfection. Depending on the severity of the ulcers, topical and/or systemic steroid agents are recommended
Parotid enlargement and dry mouth
Parotid enlargement is commonly associated with HIV infection in chidren (10%-30%) and less commonly in adults. It occurs in the late course of HIV infection and its associated with a slower rate of HIV disease progress. Parotid enlargement occurs as one side or both side swelling of the parotid glands. It is usually painless and may be accompanied by decreased salivary flow (dry mouth). Problems with dry mouth in HIV-infected patients are often caused by medications that interfere with salivary secretion, such as antihistamines, antianxiety medications, antidepressants and some antiretroviral drugs. Dry mouth can lead to dental decay, periodontal disease, oral candidiasis, mucosal injury and dysphagia, and is often associated with pain and reduced oral intake of food.
Treatment : The treatment for dry mouth focuses on symptomatic relief through hydration, mimimizing the consumption of alcohol and caffeine, and using artificial saliva. The use of pilocarpine to stimulate saliva flow may be useful option. Good oral hygiene measures and diet control (control for sugar and sugary food) are recommended to prevent dental caries. Mouth rinses with high alcohol content should be avoided due to drying effect.
References
- Denis P.Lynch. Oral manifestation of HIV disease : An update. Seminar in Cutaneous Medicine and Surgery,Vol 16.No4.1997:pp 257-264
- Laskaris G. Oral manifestation of HIV disease. Clinics in Dermatology.2000;18:447-455
- Peter H, et al. Oral manifestation in HIV-infected patients: Diagnosis and management. Journal of the American Academy of Dermatology. 1993;29:749-60.
- Hirata CHW. Oral manifestation in AIDS. Braz J Otorhinolaryngol. 2015;81:120-3.
| Last Reviewed | : | 6 October 2015 |
| Writer / Translator | : | Dr. Nor Nazaliza bt. Basri |
| Accreditor | : | Dr. Hans Prakash a/l Sathasivam |