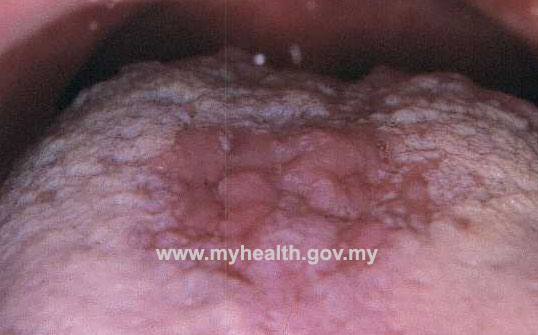
What is Oral Candidiasis?
Around half the normal population carry the fungal organism from the Candida species in their mouth without it causing any disease. Oral candidiasis is when this organism causes disease or lesions in the oral cavity. It is the most common oral fungal infection. Candidiasis typically occurs when there is either an immune defect or when the local ecology is altered/disturbed. This means that the candida organism usually requires an opportunity to cause an infection hence the term “opportunistic infection”.
Factors that increase the risk of oral candidiasis can be either local or systemic.
Local factors
- Dry mouth
- Smoking
- Corticosteroids (topical/inhalation)
- Dental appliances
- Broad-spectrum antimicrobials
- Radiotherapy
Systemic factors
- Malnutrition
- Immune defects such as:
- Diabetes mellitus
- HIV infection
- Immunosuppressive drugs etc
- Cytotoxic chemotherapy
- Anaemia
What are the Signs & Symptoms?
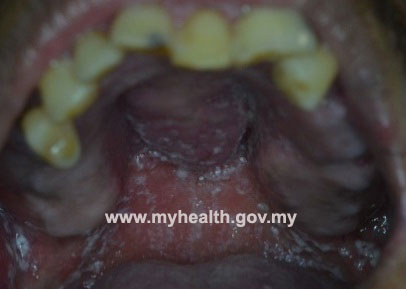
Symptomatic candidiasis presents usually as either white lesions, red lesions or mixed red and white lesions. It can cause discomfort and soreness as well as pain but at times can be painless. As such, candidiasis can present in various forms in the oral region and is usually classified according to its clinical presentation (appearance and involvement of other area of the body). The following are some of the different forms of oral candidiasis:
- Acute pseudomembranous candidiasis (Thrush)
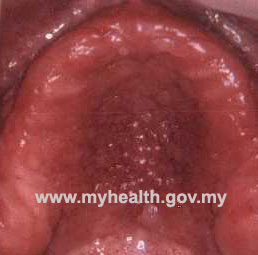
- Acute erythematous/ Atrophic candidiasis
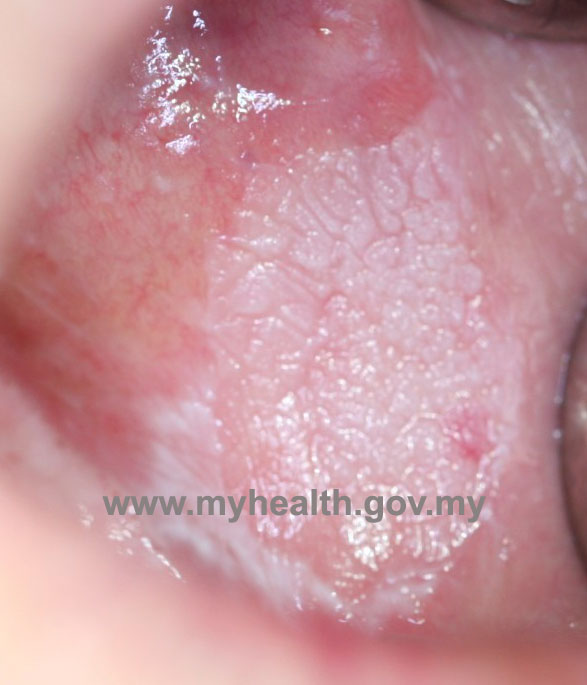
- Chronic hyperplastic candidiasis*
- Chronic erythematous / atrophic candidiasis
- Chronic multifocal oral candidiasis
- Candida-associated lesions:
- Denture related stomatitis
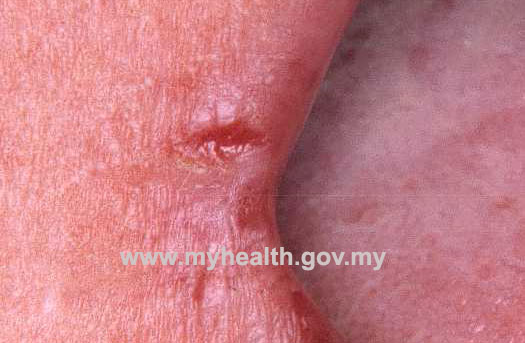
- Angular cheilitis/stomatitis
- Median rhomboid glossitis
- Oral manifestation of systemic mucocutaneous candidiasis
*Of all the different clinical presentations, chronic hyperplastic candidiasis has a potential to undergo cancerous change.
Diagnosis
Diagnosis is usually through clinical findings. However, in some cases swabs or smears will need to be performed to identify the offending organism. In cases of chronic hyperplastic candidiasis, a tissue biopsy is almost always recommended due to the potential for malignant change.
As oral candidiasis is frequently associated with systemic conditions such as diabetes mellitus, nutritional deficiencies and HIV infection, blood tests to investigate possible underlying / predisposing causes may be performed by the attending specialist.
Management
Management of oral candidiasis is very much dependent on the clinical presentation as well as possible predisposing factors. Identifying and managing an existing predisposing factor is extremely important in the management of oral candidiasis as it would help prevent prolonged and repeat treatment.
In most cases without serious underlying conditions, topical antifungal agents either in the form of lozenges, mouth rinses or gels would be prescribed by your specialist. At times, intermittent or prolonged topical antifungal treatment may be necessary when the underlying cause is unavoidable / incurable. And in cases of widespread or deep seated infection, systemic antifungals may be prescribed.
Improvement in oral hygiene measures are also advisable especially for those using dental appliances. Good oral hygiene measures can drastically reduce the amount of fungal organisms in the mouth.
References
- Samaranayake LP, Holmstrup P. Oral candidiasis and human immunodeficiency virus infection. J Oral Pathol Med 1989
- Samaranayake LP, Keung Leung W, Jin L. Oral mucosal fungal infections. Periodontol 2000 2009
- Scully C. (2008). Oral and maxillofacial medicine- The basis of diagnosis and treatment. (2nd ed.) Elsevier.
- Vazquez JA, Sobel JD. Mucosal candidiasis. Infect Dis Clin North Am 2002
| Last Reviewed | : | 11 May 2015 |
| Writer | : | Dr. Hans Prakash a/l Sathasivam |
| Accreditor | : | Dr. Lau Shin Hin |