Introduction
Cleft lip and cleft palate, previously known as hare-lip is a group of conditions that includes cleft lip, cleft palate, and both together. A cleft lip contains an opening in the upper lip that may extend into the nose. The opening may be on one side, both sides, or in the middle. A cleft palate is when the roof of the mouth contains an opening into the nose. It occurs in about 1 to 2 per 1000 births in the developed world and is due to failure of facial tissues to join together properly during development. The cause is unknown in most cases. Risk factors is associated with smoking during pregnancy, diabetes, an older aged mother, obesity, and certain medications such as some used to treat seizures. They can often be diagnosed during pregnancy with an ultrasound scan.
Unilateral cleft lip and palate is more common than bilateral cleft lip and palate which accounts for about 10% of all cases. For unknown reasons, left sided cleft is twice as common as right sided cleft of lip and palate. A cleft lip or combined cleft lip and palate are more common in boys, but a cleft palate on its own is more common in girls.
Complications
- Dental Problems Most common dental problems seen include small teeth, missing teeth, extra teeth (called supernumerary), or teeth that are out of position. They may have a defect in the bone that supports the teeth (alveolar ridge) leading to displaced, tipped, or rotated permanent teeth or even prevent permanent teeth from coming in properly.
- Speech Problems Unlike cleft palate, patients with cleft lip have fewer speech problems. Cleft palate patients often produce hypernasal sounds (sounding like air escape through the nose) and even distorted sounds, particularly “s,” “sh,” “ch,” and “j.” This happens because the palate doesn’t move well enough to prevent air from leaking out of the nose.
- Clinical problems Clinical problems encountered in treating such patients are similar to those of patients who have undergone ablative tumor surgery in the maxilla. Typical findings in adult edentulous cleft palate patients include dysphagia, leakage of oral fluids, hypernasal speech, compromised chewing ability, and aesthetic disturbances.
Treatment
A cleft lip is usually surgically repaired when a child is 3 to 6 months old. Special procedures like lip adhesion or a molding plate device is used if the cleft lip is wide. This repair usually leaves a small scar on the lip under the nose. Cleft palate is usually repaired at 9-12 months of age. The aim of surgery is to create a palate that works well for speech. More surgeries may be needed to help improve speech and provide stability for permanent teeth as the child grow older and undergo some facial changes. These surgeries are done when the child is between 6 and 10 years old. Missing permanent tooth in young cleft patients can be replaced either with a removable appliance or a dental implant.
Prosthetic rehabilitation
The prosthetic management of patients with cleft lip and palate deformities has challenged clinicians for centuries. The prosthesis constructed is meant to serve more than one purpose. The prosthetic devices must not only serve as a palatal obturator to prevent food and liquid from leaking into the nasal cavity, but it must also help to improve speech intelligibility, and provide a functional and aesthetic replacement for missing teeth and supporting tissue.
Various prosthetic choices are available ranging from a conventional to the use of osseointegrated implant. The fabrication of the appliance is not only for a more convenient wearing, but also provides greater stability, retention, and chewing efficiency. The combination of bone grafting and implant-supported fixed or removable prostheses represents an invasive treatment approach; whereas, a conventional fixed or removable prosthesis represents a more conservative alternative for patients who refuse surgical intervention.
|
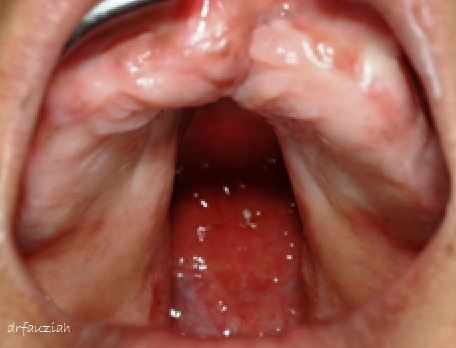
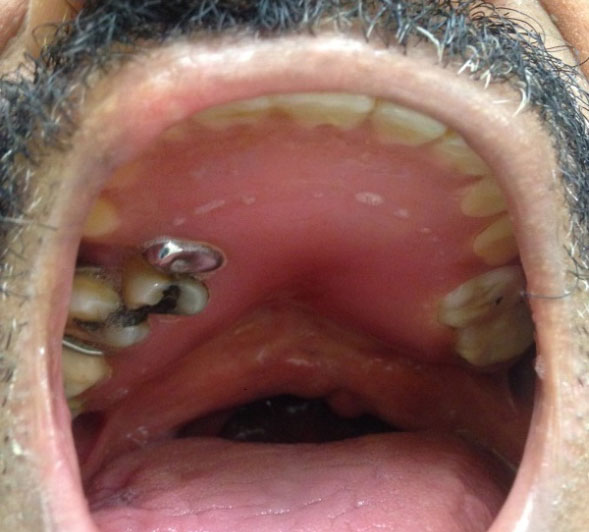
Fig. 1. Direct view of a maxillary arch with a wide cleft of the hard and soft palate.
|
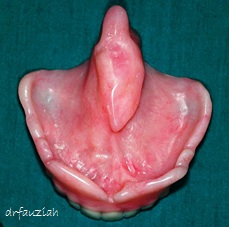
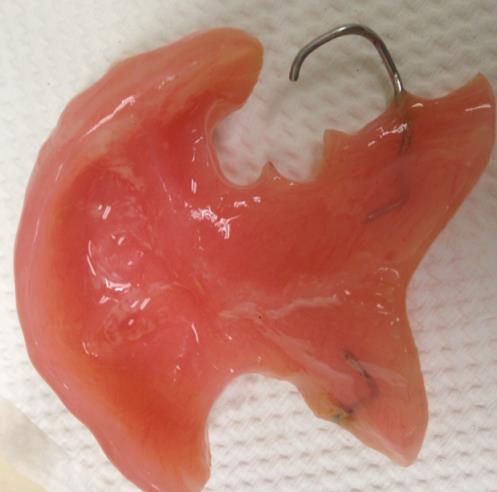
Fig. 2. View of an obturator constructed for the cleft palate patient in Fig 1.
|
|
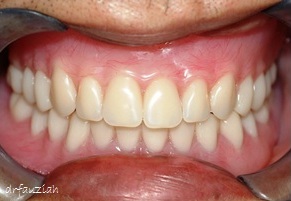
Fig. 3. Anterior view of the obturator and a lower complete denture in the mouth.
|
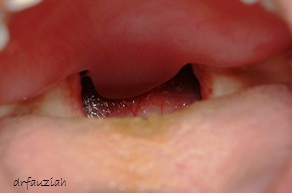
Fig. 4. Close up view of the obturator in the mouth.
|
|
Fig. 5. Another case of a cleft palate patient with an obturator constructed. The obturator will prevent food and liquid from leaking into the nasal cavity. rator in the mouth.
|
|
In an unrepaired bilateral cleft lip and palate where oronasal communication is relatively large, with the presence of hyperplastic soft tissue surrounding the hard palate defect and a severely resorbed alveolar ridge, there is a need for a combination of fixed implant-supported and removable prostheses in conjunction with an extracoronal resilient attachment for retention. A combination of metal-ceramic cement-retained fixed partial restorations and removable prosthesis will help to cover the oronasal communication in the hard palate for optimal outcome and fulfill patient’s functional and aesthetic need.
The prosthetic rehabilitation will provide the cleft lip and palate patients a more aesthetic appearance, allow patients to feel more normal, increases their self-esteem, and offers them greater opportunities for employment and fulfilling their social potential.
References
- Ayse Mese and Eylem Ozdemir. Removable partial denture in a cleft lip and palate patient: A case Report. J Korean Med Sci.2008 Oct; 23(5): 924-927 {Pubmed}
- Bora Bagis et al. Rehabilitation of a congenital palatal defect with a modified technique: a case report. Cases J. 2008; 1:39. Published online 2008 July 16. doi: 10.1186/1757- 1626-1-139.{PubMed}
- Jose Alberto et al. Rehabilitative treatment of cleft lip and palate: experience of the Hospital for Rehabilitation of Craniofacial Anomalies/USP (HRAC/USP) Part 4: Oral Rehabilitation. J Appl Oral Sci. 2013 May – Jun; 21(3): 284- 292. doi 10.1590/1679-775720130127 {PubMed}
| Last Reviewed | : | 28 August 2020 |
| Writer | : | Dr. Balkis bin Ghazali |
| Accreditor | : | Dr. Fauziah bt. Ahmad |
| Reviewer | : | Dr. Roshima bt. Mohd Sharif |