What is jaundice?
Jaundice is the yellowish discolouration of the skin caused by an increase of bilirubin in the blood.
What is bilirubin?
Bilirubin is a pigment produced from the breakdown of red blood cells. It is then processed in the liver before being passed out into the stools.
How common is jaundice in babies?
Jaundice is very common and occurs in 50% of babies in the first week of life.
What causes neonatal jaundice?
- Physiological Jaundice
Physiological jaundice is the most common cause of neonatal jaundice and is harmless to your baby. The onset of physiological jaundice is after the first 48 hours and will subside by the end of the first week of life. It is caused by the normal breakdown of red blood cells and the immaturity of the liver. As such, late preterm babies of between 34-36 weeks are at higher risk of developing jaundice if they do not receive early treatment. - Pathological Jaundice
Pathological jaundice – jaundice with onset in the first day of life is usually pathological. Causes includes:- Incompatibility between mother’s and baby’s blood group (in mothers with Rhesus negative or Blood Group O blood).
- Babies with G6PD (glucose 6 phosphate dehydrogenase) deficiency in their red cells resulting in their instability on exposure to certain agents. This occurs in less than 5% of babies. All newborns are screened for G6PD deficiency at birth.
- Infection in the newborn which makes the baby unwell and needs in-hospital treatment.
What causes jaundice in babies to be prolonged?
Jaundice is considered prolonged if persists for longer than 14 days in a term baby and 21 days in a preterm baby. Common causes are:
- Breast milk jaundice – Babies on exclusive breast feeding may have prolonged jaundice. As long as the mothers are not taking traditional herbs, the jaundice will be harmless to the babies.
- Urinary tract infection.
- Obstruction of bile flow from the liver into the intestine. This rare condition will result in pale coloured stools and dark or tea coloured urine.
- Congenital hypothyroidism – This condition occurs in 1 per 4000 babies. Currently the national screening programme of newborn cord blood for congenital hypothyroidism is an ongoing programme in all government hospitals and clinics.
Risk factors for severe Neonatal Jaundice?
- Baby born premature
- Low birth weight
- Jaundice within 24 hours of life
- Mother withblood group ‘O’ or Rhesus Negative
- G6PD deficiency
- Cephalhaematoma or bruises
- Babies of diabetic mothers
- Family history of severe NNJ in siblings
What should I do if my baby has jaundice?
Consult your doctor or health nurse for a proper evaluation. However, your baby is likely to be healthy in the following situations:
- Term baby with no risk factor for excessive red cell breakdown.
- Jaundice appearing after the first 48 hours of life and not increasing in severity.
- Healthy, active and feeding well.
What are the danger signs that I should be aware of?
You need to consult your doctor urgently in any of the following situations :
- Jaundice appearing within the first 24 hours of life.
- Rapid progression of jaundice.
- If the result of the newborn screening shows G6PD deficiency.
- If previous babies in your family have severe neonatal jaundice.
- If your baby is unwell and not feeding satisfactorily.
- If there is presence of pale coloured stools or dark or tea-coloured urine.
- Your baby is born preterm
What would the doctor do?
Your doctor will assess your baby clinically, proceed to do relevant investigations and then institute appropriate treatment. He will advise you on the specific situation of your baby.
What problems can jaundice cause?
- Acute Bilirubin Encephalopathy (ABE) changes in behaviour and muscle tone
- Kernicterus – lead to cerebral palsy and deafness and intellectual disability
Early intervention of babies at risk of severe jaundice will prevent this complication.
What are the ways to treat this condition?
There are two ways to bring down the bilirubin levels to avoid brain toxicity. These are:
- Phototherapy
- Exchange transfusion
Your baby will be put under a phototherapy light unit. The blue coloured component of the light can convert the bilirubin to a non-toxic product.
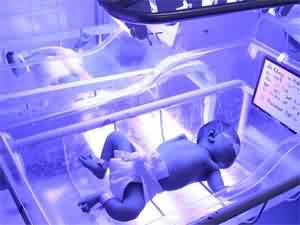
Newborn undergoing intensive phototherapy for severe neonatal jaundice.
Should not do: You should not expose your baby to sunlight for treatment due to risk of dehydration and sunburn
The toxic bilirubin level for term babies in the first week of life is usually taken as more than 20 mg/dL (340 umol/L). Exchange transfusion is used as a last resort to try to avoid brain toxicity due to severe neonatal jaundice. The levels for exchange transfusion will depend on many factors including the age of the baby and the cause of the jaundice.
Prevention
It is important to identify and monitor babies at risk of severe jaundice. Early detection of babies with jaundice needs to be done to ensure early and appropriate intervention.
What else can be done for babies who had suffered severe jaundice?
All babies with high bilirubin level (20 mg/dL or higher) should be followed up in a paediatric clinic to check on the hearing and development. Some babies may need to be referred to the audiology department for a hearing test to exclude high tone deafness.
Brain damage due to severe jaundice (kernicterus} should be prevented. If it happens, the child should be referred to a multi-disciplinary team for rehabilitation.
| Last reviewed | : | 28 August 2020 |
| Writer | : | Dato’ Dr. Jimmy Lee Kok Foo |
| Dr. Leow Poy Lee | ||
| Reviewer | : | Dr. Zainab bt. Kusiar |







