Itchy eyes are a common ocular symptom. This symptom can be associated with eye redness, frequent eye rubbing, lid swelling, photophobia and blurred vision. The commonest causes of eye itchiness are allergic conjunctivitis, blepharitis and dry eye.
Allergic conjunctivitis is an ocular surface allergic reaction towards an irritant substance called as an allergen. The patent develops an immune reaction due to hypersensitivity to the allergen. Allergic conjunctivitis can be divided into Seasonal Allergic Conjunctivitis (SAC), Perennial Allergic Conjunctivitis (PAC), Vernal keratoconjunctivitis (VKC) and Atopic keratoconjunctivitis (AKC).
The onset of symptoms in SAC is seasonal and is mainly associated with trees and pollen whereas PAC will induce symptoms throughout the year and is related mainly to dust mites, dander and feathers. Both commonly present with seasonal or perennial rhinitis as well. VKC patients present with a background history of atopy whereas AKC presents with atopic dermatitis of the lids.
The clinical signs of SAC and PAC are quite similar. These include bilateral lid swelling, conjunctival hyperemia, mild papillary reaction and chemosis. Both rarely involve the cornea. Vernal keratoconjunctivitis and Atopic keratoconjunctivitis have significant papillae over the tarsal conjunctiva and limbus (Figure 1). Both also affect the corneal surface resulting in punctate epithelial keratitis, erosions and shield ulcer if left untreated (Figure 2). At this stage, the vision will be affected.
Figure 1
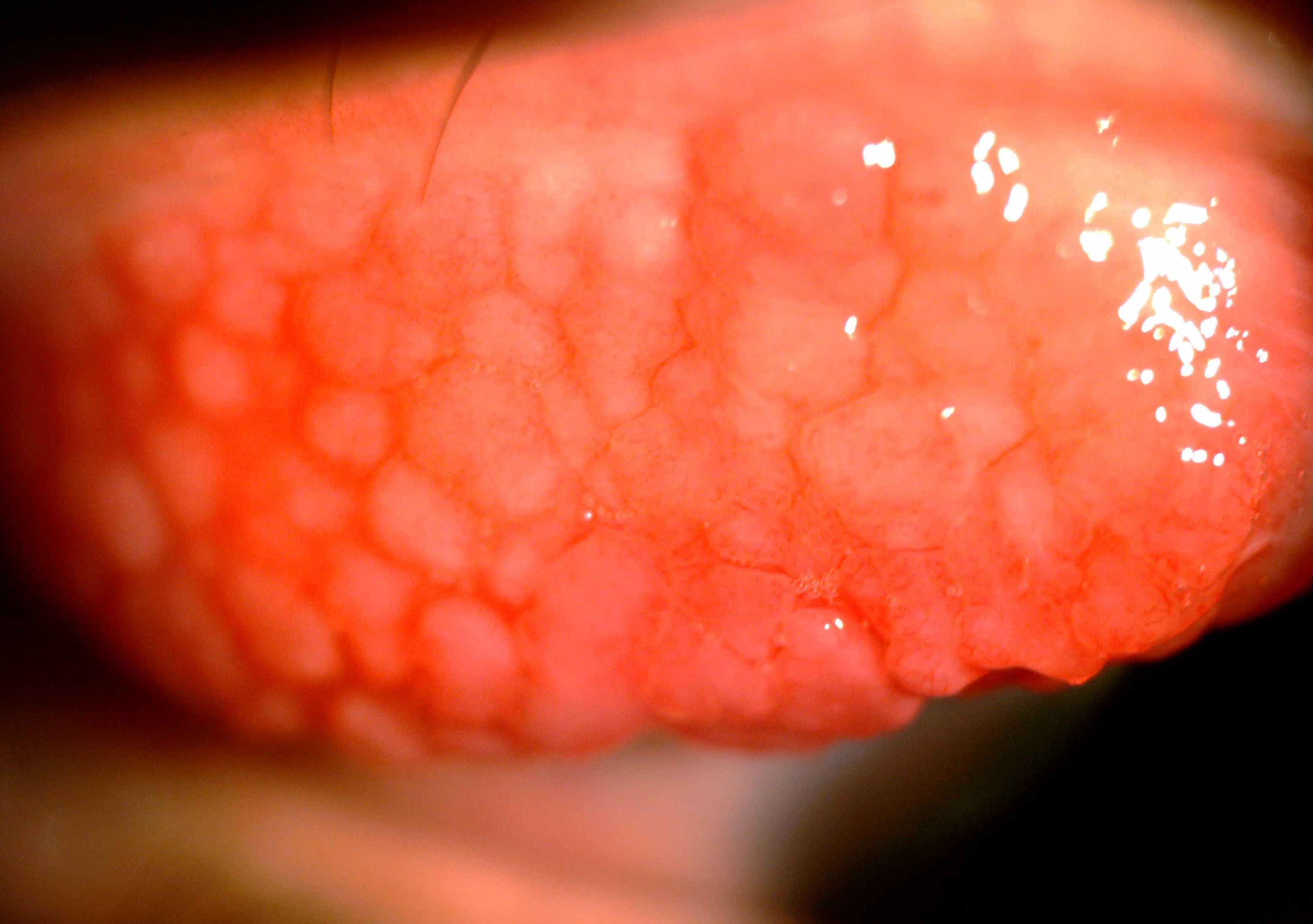 |
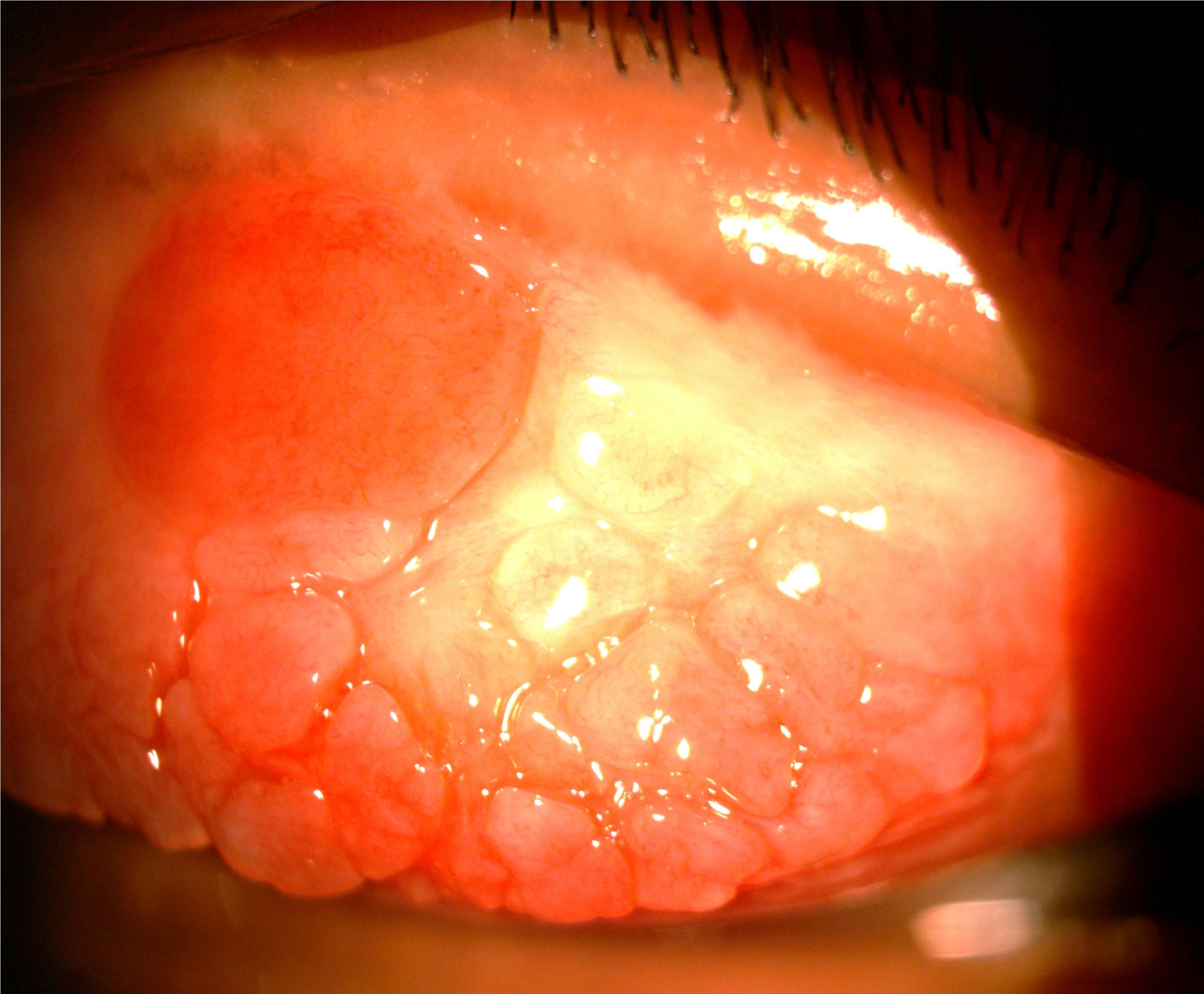 |
| Conjunctival papillae | Cobblestone conjunctival papillae |
Figure 2
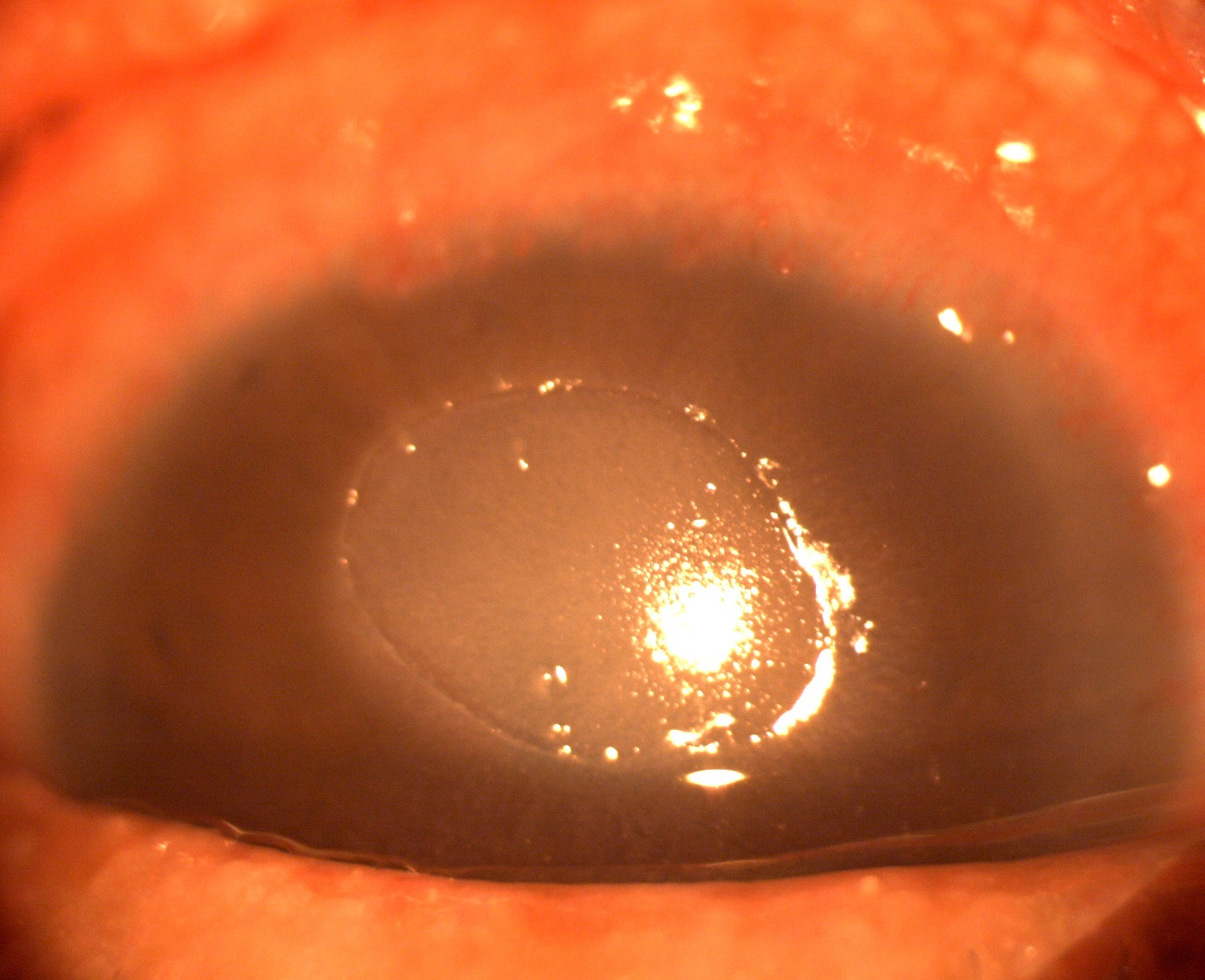 |
 |
| Corneal shield ulcer | Corneal shield plaque |
Patients with allergic conjunctivitis require skin prick test in order to identify the allergens. Patients will be advised to avoid the allergens they are sensitive to. Besides that, they are advised to stop rubbing the eyes as eye rubbing releases more histamine which will worsen the inflammation and aggravate the itchiness. Instillation of cool artificial tears helps dilute the inflammatory mediators and allergens whereas cold compression provides additional relief and reduces the swelling.
Medical therapy for allergic conjunctivitis include topical antihistamine eye drops, vasoconstrictors, mast cells stabilizer and anti-inflammatory medication. Supra tarsal injection is an option in refractory cases.
The complications of allergic conjunctivitis are mostly associated with vernal and atopic keratoconjunctivis. Healed corneal shield ulcer results in poor vision due to corneal scarring. The habit of constant eye rubbing induced by itchy eyes can cause corneal ectasia. This is a stage whereby the cornea becomes weak and thin and subsequently progresses to keratoconus. Other complications includecataract and secondary glaucoma.(Steroid responder)
Eye allergies can also be caused by reactions to certain allergens for example eye drops, cosmetics and contact lenses. The treatment is to avoid the allergens.
Blepharitis is a common chronic eyelid margin inflammation. It is commonly caused by bacterial infection or blockage of the Meibomian glands. It is divided into anterior blepharitis and posterior blepharitis. Anterior blepharitis affects the portion of the eyelid where the eyelashes are attached. Posterior blepharitis is due to dysfunction of meibomian glands within the eyelids that secrete oils to help lubricate the eye. The symptoms and signs are itchy , watery eye, redness, eye stickiness, lid margin crusting, lid swelling etc (Figure 3). The treatment includes lid hygiene, topical antibiotic, systemic antibiotic, artificial tears and topical corticosteroids.
Figure 3
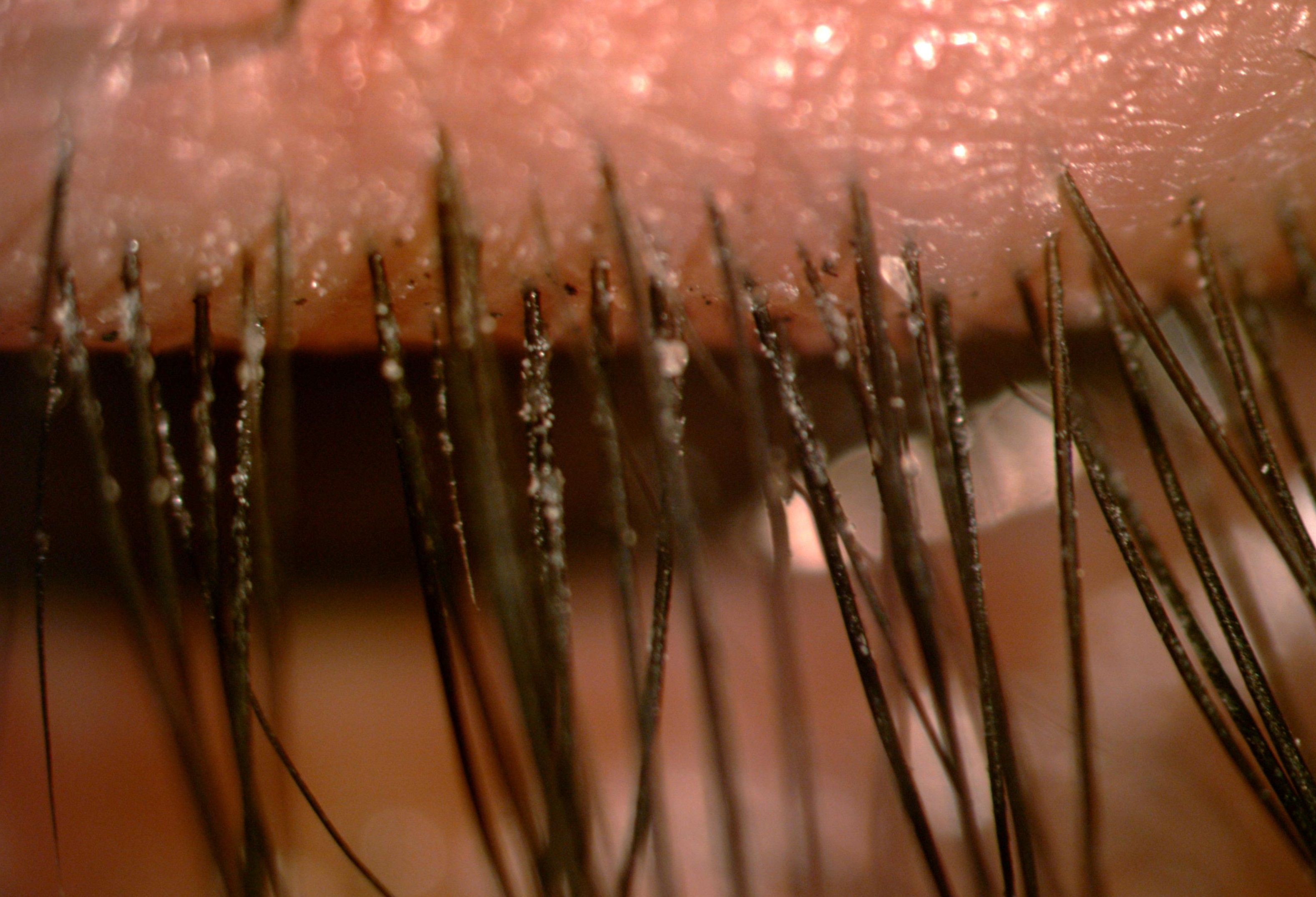 |
| Lid margin crusting in blepharitis |
Dry eyes occur when tears are not able to provide adequate lubrication for the surface of the eyes as seen in dysfunction of the lacrimal gland and Meibomian glands. Symptoms noted include itchy eyes, foreign body sensation, burning sensation, tearing and redness. Treatment of dry eye encompass tear film substitutes in the form of eye drops and ointment, anti-inflammatory eye drops and punctal occlusion.
Conclusion
Itchy eyes are an important ocular symptom. Patients need to consult an eye specialist for proper diagnosis and treatment of this symptom.
Reference
- Krachmer, Jay H. Mannis, Mark J. Holland, Edward J.Book Title: Cornea Fundamentals, Diagnosis and Management. 3rd Edition 2011
| Last Reviewed | : | 23 August 2019 |
| Writer | : | Dr. Rohana bt. Alias |
| Accreditor | : | Dr. Chandramalar a/p T Santhirathelagan |
| Reviewer | : | Dr. Rosniza bt. Ab. Razak |







