Interstitial lung disease describes a large group of disorders most of which cause progressive scarring of the lung tissue which is irreversible. The scarring of lung tissue will affects your ability to breathe and get enough oxygen into your blood. The scarring of the lung can be caused by long-term exposure to hazardous materials like asbestos and it can also be part of systemic illness like connective tissue disease but in most cases the causes remain unknown.
Interstitial lung disease is uncommon compared to other pulmonary problems and it is mainly a disease of the middle-aged and elderly.
Signs & Symptoms
The primary symptom of interstitial lung disease is shortness of breath which develops slowly over months. Most patients with interstitial lung disease will experience breathlessness which may worsen over time.
Other symptoms include cough which is usually dry and non-productive. Some people with interstitial lung disease can also have fever, weight loss and feeling tired all the time.
Causes / Risk Factors
For most types of interstitial lung disease, the cause is unknown. Some interstitial lung disease occur when you have another medical condition like rheumatoid arthritis or scleroderma.
Interstitial lung disease can be triggered by many different things including airborne toxins in the work place like asbestos, silica and radiation. Some medications can also cause damage to the lung like chemotherapy drugs, heart medications and some antibiotics.
There are certain factors that make you more susceptible to develop Interstitial Lung Disease and these include gastroesophageal reflux disease, smoking and continually inhaling very high levels of oxygen.
Tests / Diagnosis
Some of the following tests may be necessary to diagnose Interstitial Lung Disease, identify its cause and the extent of the lung damage.
- Imaging tests :
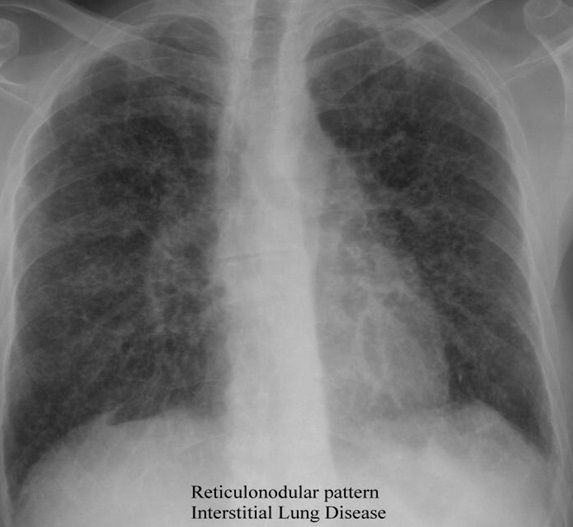
- Chest X-ray. It can be normal but often there will be a characteristic pattern on chest X-ray.
- Computerized tomography (CT) scan. A high-resolution CT scan is used to determine the extent of lung damage caused by the disease and details of fibrosis.
- Pulmonary function test :
This test measures how well you can breathe in or out and how much your lung and breathing ability have been affected. It is also used to monitor the disease progression.
- Lung biopsy :
Sometimes lung biopsy is required to get the definitive diagnosis. It can be done either through bronchoscopy or surgical biopsy.
Treatment
The lung scarring in interstitial lung disease cannot be reversed and treatment will not always be effective in stopping the disease progression. There is no approved or proven therapy that can cure interstitial lung disease. Some therapies that are used may delay the disease progression and some may improve quality of life. Patients usually will be given immunosuppressant medications like corticosteroid or azathioprine to suppress the immune system and reduce inflammation.
Oxygen therapy is required for some with low level of oxygen in the blood.
Lung transplant is an option for some advanced cases.
Complication
Interstitial lung disease may lead to the following complications :
- Pulmonary hypertension. High blood pressure in your lungs which affects the arteries in your lungs.
- Right sided heart failure (cor pulmonale). This condition is often a consequences of pulmonary hypertension.
- Respiratory failure. In the end stage of the disease, respiratory failure occurs when there is a severely low blood oxygen level together with pulmonary hypertension and right-sided heart failure.
Rehabilitation / Living
Patients with interstitial lung disease should stay as healthy as possible and they should:
- Stop smoking
- Eat well
- Get vaccinated as respiratory infections can worsen the symptoms.
Pulmonary rehabilitation is recommended to help patient achieve their highest level of function. The goals of pulmonary rehabilitation are to improve quality of life by decreasing respiratory symptoms and complications, improving physical conditioning and exercise performance, improving emotional well-being and reducing hospitalizations. The program includes education, exercise conditioning, breathing techniques, nutritional counselling and psychosocial support.
| Last Reviewed | : | 29 May 2017 |
| Writer | : | Dr. Rozanah bt. Abd Rahman |
| Accreditor | : | Dr. Jamalul Azizi b. Abdul Rahman |







