It is one of the most common women’s gynaecologic disorders. Nearly one in seven women of the reproductive age group mainly between 30 and 45 years old, are affected by it.
This is a non-cancerous condition found in women where some of the tissues that line the inside of the womb are found elsewhere in the human body such as the pelvis where the bladder, intestines and female reproductive organs are found. Commonest sites are the ovaries and the posterior ligaments that support the uterus.
The exact cause of the disease remains unclear. The most common theory is referred to as ‘retrograde menstruation’, where a portion of the menstrual blood flows backward into the peritoneal cavity through the fallopian tube. The endometrial cells are thought to attach themselves into the various locations in the pelvic cavity.
The following may occur in the women with endometriosis:
- Heavy and sometimes irregular periods
- Painful periods
- Pain during sex
- Pain in the pelvis or lower abdomen in between periods
- Endometriosis may also affect a women’s ability to get pregnant.
However, some women with endometriosis may experience no symptoms. It is important to note that the amount of pain is not related to the extent of a patient’s endometrial growths. Some women with numerous growths have no pain while others with minimal endometriosis experience severe pain.
During menstruation endometrial growths can bleed, just like the uterine lining bleeds in response to the hormones of menstrual cycle. However, unlike the lining of the uterus, products of the endometrial growths have no way of leaving the body. If a women becomes pregnant or enters menopause, the endometrial growths shrink and much of the pain is eliminated.
This problem can be suspected after the doctor has taken a careful medical history and medical examination including a pelvic examination. It is most accurately diagnosed from laparoscopy (key-hole surgery) when special instruments are used to look for these tissues in your pelvis. Treatment however, can be started without the need for confirmation by laporoscopy.
Treatment either medical or surgical depends on the kind of problems a patient is experiencing. The objective would be either of the following;
- relieving pain and other symptoms
- halting the progression of the future lesions
- restoring fertility to those patients who have lost the ability to become pregnant, and
- preserving reproductive function for the future childbearing.
The medical treatment of endometriosis is directed at suppressing woman’s levels of estrogen and progesterone, which stimulate the endometrial growths. Traditionally used drugs are oral contraceptive pills, high doses of progesterones, and male hormone derivatives example danazol.
Other medical treatment option would be GnRH (Gonadotropin-Releasing Hormone) analogues. These are monthly or 3 monthly injections, which interrupt the production of estrogen therefore producing a medically-induced menopause. The usual duration would be up to six months. The side effects include hot flushes, decreased libido, and vaginal dryness. A small amount of bone loss may also occur during therapy, but this is partially or completely recovered once treatment has stopped.
It must be remembered that there is a significant recurrence rate of disease after medical treatment. Therefore maintenance therapy is required for those women who are not embarking on a pregnancy following medical treatment.
Diegonest is a new drug that can be used for long term maintenance therapy to reduce risk of progression or recurrence of endometriosis.
Surgical treatment could either done via laporoscope or open surgery. It could be reconstructive (removal of endometriosis and repair of the affected organs) where fertility needs to be preserved. Clearance surgery involving removal of ovary, womb and other endometriosis deposit may be indicated if all options had failed.
Endometriosis affects each individual differently. Ultimately the choice of treatment for endometriosis has to be individually tailored to the needs of the patient.
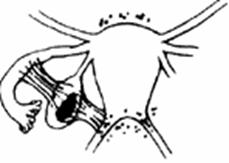
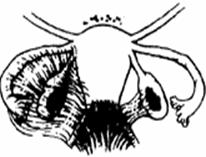
| Stage I (Mild) | Stage II (Moderate) |
|---|---|
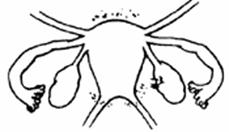 |
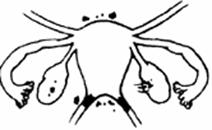 |
| Stage III (Mid) | Stage III (Mid) |
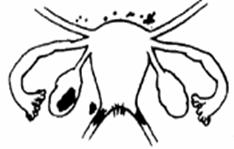 |
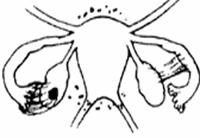 |
| Stage IV (Severe) | Stage IV (Severe) |
 |
 |
| Last Reviewed | : | 23 August 2019 |
| Writer | : | Dr. Kannappan a/l AL Palaniappan |
| Accreditor | : | Dr. K.K Iswaran |
| Reviewer | : | Dr. Rafaie bin Amin |







