Definition
Anaemia is a condition where the number of red blood cells (RBCs) or haemoglobin within those cells in the blood is lower than the normal range. Oxygen binds to haemoglobin, the main part of a red blood cell (RBC), and gets carried away from the lungs to other organs and tissues in the body. Anaemic patients often present with symptoms including fatigue, paleness and persistent shortness of breath as the organs are not getting enough haemoglobin and thus oxygen to function properly.
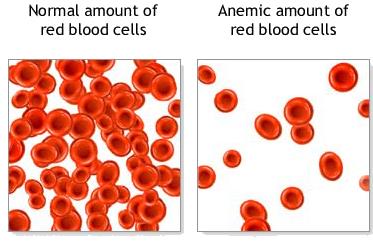
(Source: http://www.pkdiet.com/pkdanemia.php)
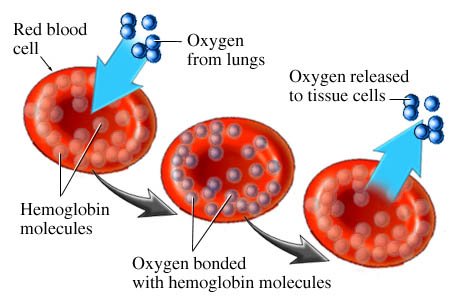
(Source: http://www.nucleusinc.com)
The causal factors of anaemia include:
- blood loss (during menstruation)
- faulty red blood cell (RBC) production and repeat destruction of red blood cell (RBC)
- pregnancy (when there is an increase in blood supply to the baby)
- hereditary traits
- poor diet; low iron, folic acid and vitamin B12 intake
There are several types of anaemia of which causes are described as follows:
- Iron Deficiency Anaemia (IDA) : due to shortage of iron causing insufficient production of haemoglobin.
- Vitamin deficiency anaemia : due to insufficient amount of folate and vitamin B12 to produce healthy red blood cells (RBC).
- Anaemia of chronic diseases : chronic diseases such as cancer and HIV/AIDS can interfere with iron level and consequently haemoglobin level thus lowering the production of red blood cells (RBC).
- Aplastic anaemia : decrease in the bone marrow’s ability to produce red blood cells (RBC).
- Anaemia associated with bone marrow disease : diseases such as leukemia and multiple myeloma can affect blood product in the bone marrow.
- Haemolytic Anaemia : red blood cells (RBC) are easily destroyed and removed from the blood stream; this can be hereditary.
- Sickle cell anaemia : The sickle-shaped RBCs die prematurely which can lead to chronic shortage of red blood cells (RBC).
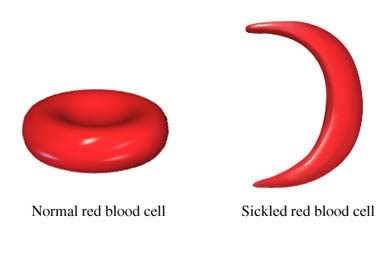 (Source: http://highschoolsicklecellanemia.weebly.com/circulatory-system.html)
(Source: http://highschoolsicklecellanemia.weebly.com/circulatory-system.html) - Other anaemias such as Thalassemia : due to defective haemoglobin; this condition can be inherited.
Parameters in blood examination in diagnosing anaemia
The methods used in measurement
A blood test can be carried out to diagnose anaemia:
- A routine haematology testing using full blood count (FBC) test can be used to determine haemoglobin, haematocrit and red blood cells (RBC) level. The haemoglobin is measured using haematology analyser which consists of SLS-haemoglobin method that combines the advantages of cyanmethaemoglobin and oxyhaemoglobin method.
- Apart from that, serum or plasma specimen can be sent to chemical pathology laboratory to measure:
- iron level where the measured serum iron concentration is principally the iron (Fe III) bound to serum transferrin.
- iron binding capacity (IBC) level which is usually known as UIBC (unsaturated iron binding capacity) and TIBC (total-iron binding capacity); UIBC measurement can be used in conjunction with serum iron concentration to obtain total-iron binding capacity (TIBC) (Iron + UIBC = TIBC).
- serum ferritin level.
- serum folate level.
- serum vitamin B12 level.
Iron and IBC level are determined by chemistry analyser with photometric colour test principle whereas the Ferritin, Folate and VitB12 are measured by using immunoassay analyser.
The reference range
The table below shows the parameters’ reference ranges for adult males and females.
|
Parameters
|
Unit
|
Male
|
Female
|
|---|---|---|---|
| Red Blood Cells |
1012/L
|
4.5 – 5.5
|
3.8 – 4.8
|
| Haemoglobin |
g/L
|
130 – 170
|
120 – 150
|
| Ferritin |
µg/L
|
22 – 322
|
10 – 291
|
| Iron |
µmol/L
|
12.5 – 32.2
|
10.7 – 32.2
|
| UIBC |
µmol/L
|
27.8 – 63.6
|
|
| Vitamin B12 |
pmol/L
|
156-672
|
|
| Folate |
nmol/L
|
> 12
|
|
Factors affecting the measurement
There are several possible sample interferences which might report a high haemoglobin concentration such as the presence of abnormal protein, leukocytosis (> 100,000/ul) or lipemic samples.
Lipemic and haemolysed samples should be avoided when analyzing the specimen because this could lead to false results.
Sample stability
The venous blood sample for FBC testing should be mixed with an anticoagulant such as EDTA-2K, EDTA-3K, or EDTA-2Na to prevent haemolysis and platelet aggregation. The sample should be analysed within 4 hours after collection and remain stable for 7 days if stored at 2-8 ºC.
Iron and IBC specimen are stable in serum and plasma for 3 weeks when stored at 2-8 ºC and 7 days when stored at 15 -25 ºC.
Ferritin, Folate and Vitamin B12 are stable for 3 weeks in serum if the sample is tightly capped and refrigerated at 2-8 ºC and up to 30 days at -20 ºC.
Interpretation
The haemoglobin, haematocrit and red blood cell (RBC) levels are found to be reduced in anaemic patients.
Serum iron concentration is decreased in iron-deficiency anaemia but increased in acute leukemia and thalassemia. TIBC is increased in iron deficiency anaemia.
Low ferritin level indicates iron deficiency anaemia and anaemia of chronic infection, while higher ferritin level from the reference range shows iron overload, thalassemia, or the patient is possibly undergoing a therapy with iron supplements.
Low folate level is a sign of macrocytic anaemia whereas low Vitamin B12 is a sign of pernicious anaemia.
Service availability
All hospitals offer full blood count testing 24 hours a day because it is a routine haematology testing in contrast to ferritin, folate and vitamin B12 which are offered only during office hours in just a few state hospitals.
Video
- https://www.youtube.com/watch?v=VkN_JVQ68Ms
- https://www.youtube.com/watch?v=IfmJeWW4OyQ
- https://www.youtube.com/watch?v=pGTu2aDbLpg
References
- page 9.2 of Chapter 9; Analyzing samples and page 15.2 and 15.4 of Chapter 15; Technical Information XN-1000 Instruction for use guidelines; Sysmex Corporation, Kobe Japan, version Feb 2011
- Clinical Chemistry Reagent Guide for Iron and UIBC of AU series of Olympus
- COBAS Ferritin, Folate, VitB12, Reagent insert and Cobas 6000 User Operation Manual
- Dacie and Lewis 2012 ‘Practical Haematology Eleventh Edition Book’
- Anemia. Understanding Anemia- The Basics, WebMD, http://www.webmd.com/a-to-z-guides/understanding-anemia-basics/. Accessed Sep 12, 2015
- Diseases and Conditions Anemia, Mayo Clinic http://www.mayoclinic.org/diseases-conditions/anemia/basics/definition/con-20026209/. Accessed Sep 13, 2015.
- Anemia, MedicineNet http://www.medicinenet.com/anemia/article.htm/. Accesed Sep 13, 2015
| Last Reviewed | : | 02 January 2017 |
| Writer | : | Faraziela bt. Abu Bakar |
| Accreditor | : | Robiah bt. Ahmad |







