Introduction
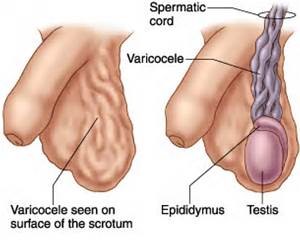
A varicocele is an enlargement of the veins within the loose bag of skin in the scrotum. A varicocele is similar to a varicose vein that can occur in your leg. They can be found in 15 percent of the general male population and 40 percent with known infertility.
Varicoceles are a common cause of low sperm production and decreased sperm quality, which can cause infertility. However, not all varicoceles affect sperm production. Varicoceles can also cause testicles failed to develop normally or shrink.
Causes
There are no known risk factors for developing varicocele. However, being overweight may increase your risk.
Your spermatic cord carries blood to and from your testicles. It’s not certain what causes varicoceles. However, many experts believe varicocele happens when the valves inside the veins that are not functioning properly thus making the blood flow to the opposite direction. The impact of the irregularity causes the veins to widen (dilate). Varicoceles may keep the local temperature in or around the testicle too high, affecting sperm formation, movement (motility) and function. This may then result in damage to the testicle and reducing the sufferer’s fertility.
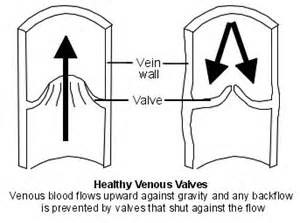
Varicoceles often formed during puberty. Varicoceles usually occur on the left side, most likely because of the position of the left testicular vein. However, a varicocele in one testicle can affect sperm production to both testicles.
Symptoms and Implications towards Fertility
A varicocele often produces no signs or symptoms. Rarely, it may cause pain. The pain may :
- Vary from sharp to dull discomfort
- Increase with standing or physical exertion, especially over long periods
- Worsen over the course of a day
- Be relieved when you lie on your back
With time, varicoceles may enlarge and experience a lump in one of your testicles or swelling in your scrotum. The varicocele is often described as looking like a “bag of worm”.
A varicocele may cause :
- Shrinkage of the affected testicle (atrophy)
The bulk of the testicle comprises sperm-producing tubules. When damaged, as from varicocele, the testicle shrinks and softens. It’s not clear what causes the testicle to shrink, but the malfunctioning valves allow blood to pool in the veins, which can result with increased pressure in the veins and exposure to toxins in the blood that may cause testicular damage.
- Infertility
Varicoceles may keep the local temperature in or around the testicle becoming too high, affecting then sperm formation, movement (motility) and function.
Diagnosis
The condition is usually diagnosed after a physical exam by your doctor. You will be examined while lying down or standing up. This is because the varicocele may not be able to be felt or seen when you lie down. If you have a smaller varicocele, your doctor may ask you to stand, take a deep breath and hold it while you bear down (Valsalva maneuver). If the physical exam is inconclusive, your doctor may order a scrotal ultrasound. In certain cases, further imaging may be recommended to rule out other causes for the varicocele, such as a tumor compressing the spermatic vein.
Varicocele Repair and Treatment
Varicocele treatment may not be necessary. However, if your varicocele causes pain, testicular atrophy or infertility or if you are considering assisted reproductive techniques, you may want to undergo varicocele repair.
The purpose of surgery is to seal off the affected vein to redirect the blood flow into normal veins. In cases of male infertility, treatment of a varicocele may improve or cure the infertility or improve the quality of sperm if techniques such as in vitro fertilization (IVF) are to be used.
Varicoceles typically develop in adolescence and likely result in worsened sperm production. Despite the decreased sperm quality overall, many men with varicoceles continue to have sufficient sperm quality to achieve a pregnancy later in life.
Clear indications to repair a varicocele in adolescents include progressive testicular atrophy, pain or abnormal semen analysis results. Although treatment of a varicocele generally improves sperm characteristics, it is not clear if an untreated varicocele leads to progressive worsening of sperm quality over time.
Varicocele repair presents relatively few risks, which may include :
- Build-up of fluid around the testicles (hydrocele)
- Recurrence of varicoceles
- Testicular atrophy
- Infection
- Damage to an artery
Repair methods include :
- Open surgery
This treatment is usually done on an outpatient basis, during a general or local anesthetic. Commonly, your surgeon will approach the vein through your groin (inguinal or subinguinal), but it’s also possible to make an incision in your abdomen or below your groin. The veins that produce the varicocele are identified and cut to eliminate blood flow to the varicocele.
Advances in varicocele repair have led to a reduction of post-surgical complications. One advance is the use of the surgical microscope, which enables the surgeon to see the treatment area better during surgery. Another is the use of Doppler ultrasound, which helps guide the procedure.
You may be able to return to normal, non-strenuous activities after two days. If you are still uncomfortable, you may do more strenuous activity, such as exercising, after two weeks. Pain from this surgery is generally mild but may continue for several days or weeks. Your doctor may prescribe pain medication for a limited period after surgery. After that, your doctor may advise you to take painkillers to relieve discomfort.
Your doctor may advise you not to have sex for a period of time. Most often, it will take several months after surgery before improvements in sperm quality can be seen with a semen analysis. This is because it takes approximately three months for new sperm to develop.
Open surgery using a microscope and subinguinal approach has the highest success rates when compared with other surgical methods.
- Laparoscopic surgery
Your surgeon makes a small incision in your abdomen and passes a tiny instrument through the incision to see and repair the varicocele. This procedure requires general anesthesia.
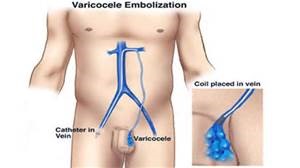
- Percutaneous embolization
This procedure is done during local anesthesia on an outpatient basis. A radiologist inserts a tube into a vein in your groin or neck through which instruments can be passed. Viewing your enlarged veins on a monitor, the doctor releases coils or a solution that causes scarring to create a blockage in the testicular veins, which interrupts the blood flow and repairs the varicocele.
This procedure isn’t as widely used as surgery.
| Last Reviewed | : | 14 April 2016 |
| Writer | : | Dr. Mohd Nasir Tak Abdullah |
| Accreditor | : | Dr. Wan Abu Bakar B. Yusof |







