Introduction
Skin cancers are uncontrolled growths of skin with presence of abnormal (malignant) skin cells. There are different types of skin cancers arising from various layers of the skin. The three main type of skin cancer are: basal cell carcinoma (BCC), squamous cell carcinoma (SCC) and malignant melanoma. Melanoma is the most dangerous skin cancer which can grow rapidly and spread to other organs.
Risk factors
There are many risk factors to the development of skin cancer in a patient. These include:
Overexposure to ultraviolet (UV) light
This is the primary cause of skin cancers. Overexposure to ultraviolet (UV) light may damage the DNA resulting in skin cancer. Repeated exposure to both UVA and UVB over long period of time from natural sunlight or artificial UV exposure are associated with increased risk of developing skin cancers.
Skin types
Those with very fair skin complexion that burn easily after sun exposure have increased risk of developing skin cancer
Genetic predisposition
There are some inherited skin diseases that make a person highly sensitive to sunlight. One example is xeroderma pigmentosum. This is an inherited skin disease in which a patient is unable to repair the damaged DNA from sun exposure. These patients are very sensitive to sunlight and often burns with minimal sun exposure. They tend to develop freckles at young age and are prone to skin cancers. Fortunately, these inherited diseases are rare.
Immunosuppression
Patient on long term immunosuppressant after organ transplant have increased risk of skin cancers
Human Papilloma virus (HPV)
This viral infection is believed to play a predominant role in the development of SCC of the penis and vulva
Exposure to arsenic and radiation
Long term exposure to chemical such as arsenic can increase the risk of getting SCC. Due to natural geological contamination, high levels of arsenic can be found in drinking water that has come from deep drilled wells. Other sources of arsenic poisonings are from traditional medicine. Exposure to radiation also increase the risk of developing skin cancer.
Smoking
Smoking tobacco has been associated with increased risk of skin cancer
Chronic non-healing wounds
Chronic non-healing wounds and long standing scars seem to predispose to the development of SCC
Symptoms
The most common sites of skin cancers are the face, head, neck, arms and back. These are due to direct sun exposure on the uncovered parts of the body. Skin cancers may have different types of appearance depending on its type. These include changes in the skin that do not heal, ulceration, discoloration and changes in the existing moles. Basal cell carcinoma (Figure 1) may start as a small, round or oval spot before growing into a raised spot with ‘rolled’ edge. It may bleed from the center and develops into a rodent ulcer. Squamous cell carcinoma (Figure 2) is pink, irregular in shape with hard surface. They can be painful to touch and sometimes ulcerate. The edges are sometimes raised. Melanoma (Figure 3) is mostly dark or black in color although sometimes it can be light brown. The surface is usually raised and rough. In the early stages, it may look like moles but with irregular borders and different shades of color in it. It has asymmetrical appearance and often larger than 6mm in diameter. Sometimes, it can bleed and becomes oozy or crusty.
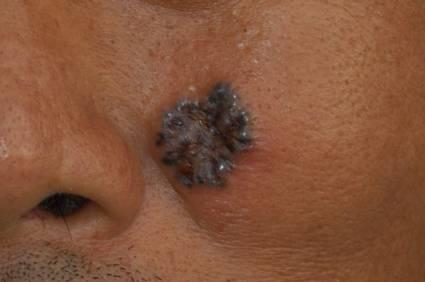 |
Figure 1: Basal cell carcinoma Raised hyperpigmented lesion on the cheek |
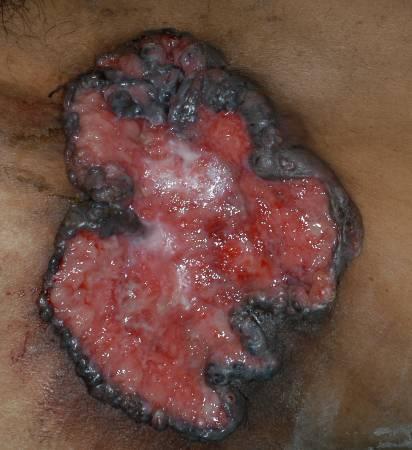 |
Figure 2 : Squamous cell carcinoma Large irregular ulcer with raised edges on the groin |
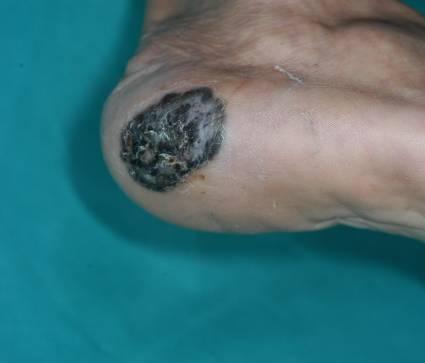 |
Figure 3 : Melanoma Irregular black nodule on the sole |
Diagnosis
Diagnosis of skin cancers rely on its clinical presentations and further confirmation by histopathological examination from skin biopsy. Therefore, any skin lesions suspicious of skin cancers should be looked into by physician immediately. Your doctor will then take a small piece of the affected skin to be sent for histopathological examination under microscope.
Treatment
Treatment is dependent on the type of skin cancer, its location, extent of lesion, age of patient, and whether the cancer is primary or a recurrence. It often involves a multi disciplinary team of dermatologist, surgeon and oncologist to decide on the best available treatment for the patient.
Surgical treatment with a wide margin for local excision can be done for basal cell carcinoma. This involves removing the cancer and a small amount of surrounding tissue. If a tumor is difficult to be completely excised due to its location, radiotherapy can be used. Other treatment options reported includes cryotherapy, topical chemotherapy (topical imuquimod or 5-fluorouracil)l and topical photodynamic therapy.
For squamous cell carcinoma arising from the skin, the tumor can be removed surgically if it is resectable. Radiotherapy is indicated for non-resectable tumor.
As melanoma can grow rapidly and spread into nearby tissues such as lymph nodes and internal organs, patients will require a complete staging by radio imaging and lymph node biopsy. If there is no spreading, the tumor can be removed surgically with wide excision margin. When a melanoma has spread, chemotherapy can be used though it is not usually effective.
Prevention
It is impossible to completely eliminate the skin cancer. We can however reduce the risk of developing such a cancer with the following measures:
- Minimizing sun exposure especially those with fair skin complexion
- Avoiding sun exposure during the peak UV times during the day, typically from 9 am to 3 pm when the sun is directly overhead
- Protect your skin by wearing protective clothing (long sleeves shirts and hats) when doing outdoors activities under sun exposure
- Using a broad-spectrum sunscreen with SPF of at least 30 that blocks both UVA and UVB radiation. Apply at least one hour before sun exposure and reapply frequently.
Outlook (Prognosis)
The outlook depends on a number of factors, including the type of cancer and how quickly it was diagnosed. Basal cell carcinoma and squamous cell carcinoma rarely spread to other parts of the body and generally has better outlook. However, melanoma is more likely to spread and has a poor prognosis if detected late.
References
- Rook, Wilkinson, Ebling. Textbook of Dermatology. Vol 4, Sixth edition.
- Igal L. Elbovitch et al. Basal cell carcinoma treated with Mohs surgery in Australia. Experience over 10 years. J Am Acad Dermatology Sept 2005;445-451
- Michael Veness et al.Role of modern radiotherapy in treating skin cancer. Australian Journal of Dermatology 2003;44,159-168
- Motley, Kersey, Lawrence. Multiprofessional guidelines for the management of the patient with primary cutaneous squamous cell carcinoma. British Journal of Dermatology 2002; 146: 18-25.
- Telfer, Colver, Bowers. Guidelines for the management of basal cell carcinoma. British Journal of Dermatology 1999; 141: 415-423.
- Preston, Stern. Nonmelanoma cancers of the skin. N Engl J Med 1992 Dec 3; 327(23): 1649-62.
- UK Guidelines for the management of cutaneous melanoma. BJD 2002; 146: 7-17
- Surgical treatment of melanoma BJD 2003;149:2-12
| Last Reviewed | : | 23 August 2019 |
| Writer | : | Dr. Ng Ting Guan |
| Accreditor | : | Datin Dr. Asmah bt. Johar |
| Reviewer | : | Dr. Nazatul Shima bt. Abd Rahim |







