What is Jumper’s Knee?
Jumper’s Knee is a clinical diagnosis of pain and dysfunction in the patella tendon. Jumper’s Knee is an overuse injury that typically has a gradual onset of pain.
It clinically presents as localised pain over along soft structure just below of our kneecaps (patella tendon). The term tendinopathy will be used in this article to mean painful tendon. This condition affects the health and quality of life by limiting sports and active participation in recreational.
Who is prone to suffer with Jumper’s Knee?
- Athletes. The prevalence was substantially higher in elite athletes (Zwerver J, 1988).
- Type of sport performed. The highest prevalence in recreational athletes was in volleyball players (14.4%) and the lowest was in soccer players (2.5%) (Zwerver J, 1988).
- Overload. A person who perform activity above what his/her tendon has adapted to at that point in time.
- Energy storage loading and jumping loading. Non-energy-storage loading or non-jumping activity (cycling & swimming) and repetitive low loading (runners) rarely aggravate the Jumper’s Knee compare to jumping and change direction task (volleyball & badminton).
What are the symptoms in Jumper’s Knee?
- Pain during a loading task such as jumping and changing direction.
- Pain during daily activity. Stairs and squatting are provocative.
- Rarely complain of night pain and morning stiffness (unless symptoms are severe)
What are the signs in Jumper’s Knee?
- Wasting of the thigh and calf muscles.
What are the complications of Jumper’s Knee?
- Patella tendon rupture. However, is rare. The majority patella tendon ruptures that do occur are in the older population (mean age 65 years) (Kannus P & Natri A, 1990).
Risk and associated factors
The factors can be divided into extrinsic and intrinsic.
- Extrinsic factors
Most commonly affect by athletes’ training environment such as:
- Increase in training volume and frequency
This is the most common factor that triggers Jumper’s Knee.
Prevalence of obesity increased with ages. 4.4% obese and 16.6% overweight adults in Malaysia are aged > 18 years.
- Change in surface density
Harden surfaces can increase Jumper’s Knee symptoms.
- Shock absorption
Amount of shock absorption in both the shoes may be vulnerable when training on hard floors or surface.
2. Intrinsic factors
- Gender
Boys and men are two to four times more likely to develop Jumper’s Knee than girls (Visnes H & Bahr R., 2013).
- Weight and height
Athletes with Jumper’s Knee were generally taller and weighed more than those without Jumper’s Knee (Zwerver J, 1988).
Different lower limb kinematics and muscle recruitment also associated with Jumper’s Knee as below:
- Thigh muscle length and strength
Shorter or less extensible quadriceps and hamstrings has been associatedwith Jumper’s Knee while greater strength has been associated with reduced pain and
improved function (Crossley KM et. al., 2007).
- Foot arch height
Lower foot arch increased Jumper’s Knee symptoms (Crossley KM et. al., 2007).
- Ankle range of motion
Reduced ankle dorsiflexion (ankle pointing downward) been associated with Jumper’s Knee (Malliaras P., 2006)
- Waist circumference
Increased waist circumference is associated with greater prevalence of Jumper’s Knee (Malliaras P, Cook JL., 2007).
What are the quick tests for Jumper’s Knee?
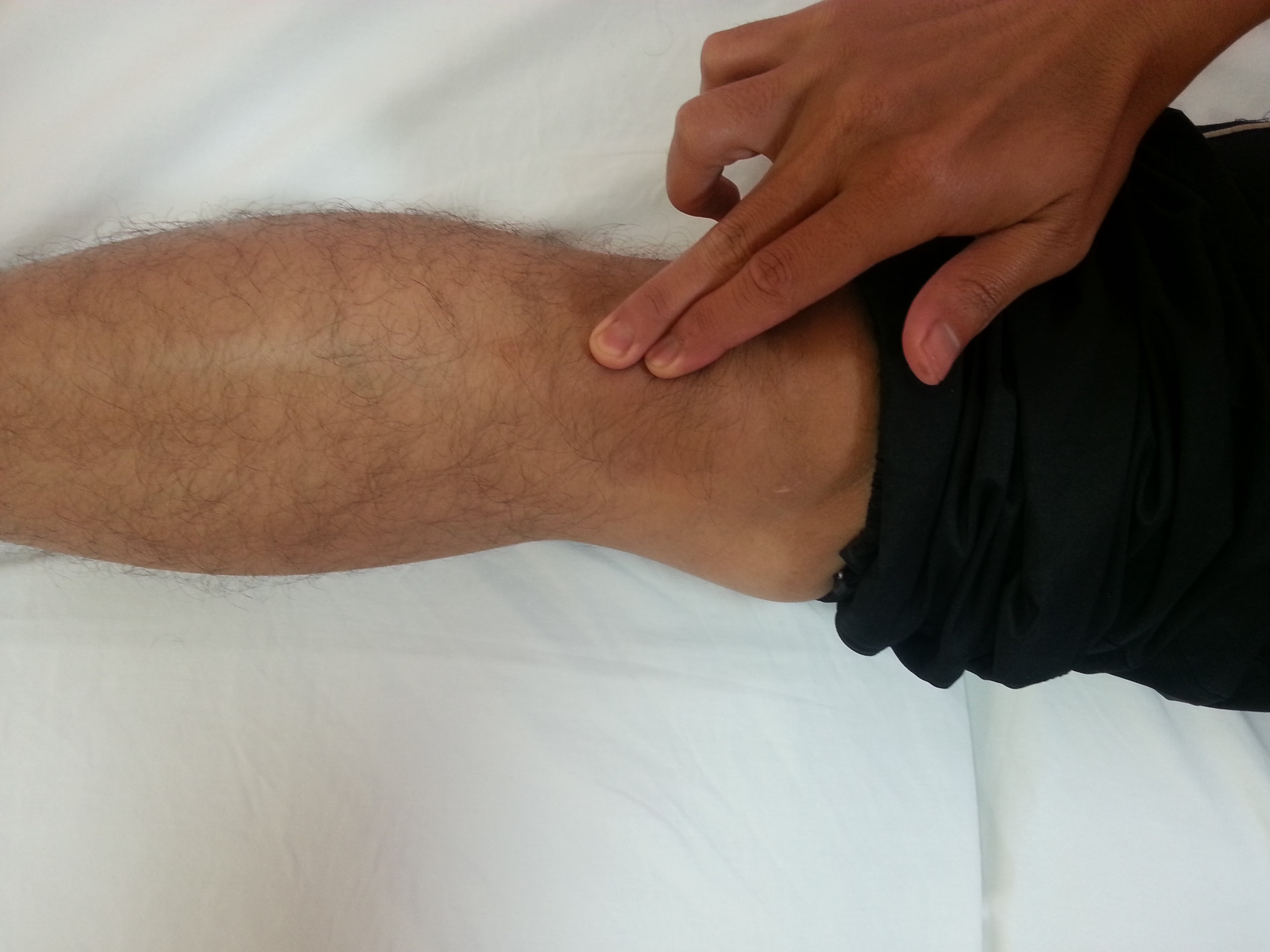
- Palpable pain along the tendon by pointing with one finger to the kneecap’s attachment.
 |
|
Instruction Position : Long sitting Action : Palpate along affected kneecap lower tendon |
| Picture 1 |
Source: Unit Fisioterapi Hospital Melaka
- Single-leg decline squat.
 |
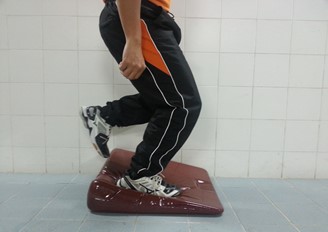 |
| Instruction Position : Standing affected leg on decline board Action : Squatting slowly Positive sign: Sharp pain along affected kneecap lower tendon |
|
| Picture 2 | |
Source: Unit Fisioterapi Hospital Melaka
- Kinetic chain function (eg Single-Leg hop test)
 |
 |
|
Instruction Position : Standing on affected leg Action : Hop forward as far as you can Positive sign: Sharp pain along affected kneecap lower tendon |
|
| Picture 3 | |
Source: Unit Fisioterapi Hospital Melaka
Physiotherapy management of Jumper’s Knee
While Jumper’s Knee may not ever completely resolve, symptoms of Jumper’s Knee can be generally managed by Physiotherapy intervention as follow:
- Passive interventions
- Load management without resorting to complete rest
- Avoid complete cessation of tendon loading activities
- Removing high-load drills from training
- Reducing frequency of training (twice per week is tolerable)
- Reducing the time of training
- Pain relief
- Heat modalities, cold therapy, pulsed ultrasound and shockwave therapy showed better outcomes in relieving pain
- Bracing and taping techniques
- Are often used clinically to help unload the patella tendon, however, no evidence supports their efficacy.
- Manual therapy techniques
- Transverse friction massage had the best effects in the short and long term (Stasinopoulos D. et. al., 2004)
- Manipulation of the knee extensor muscle group, have had a positive effect on reducing pain in Jumper’s Knee patients in short and long-term follow-up (Pedrelli A, Stecco C & Day JA., 2009)
- 2.Active interventions
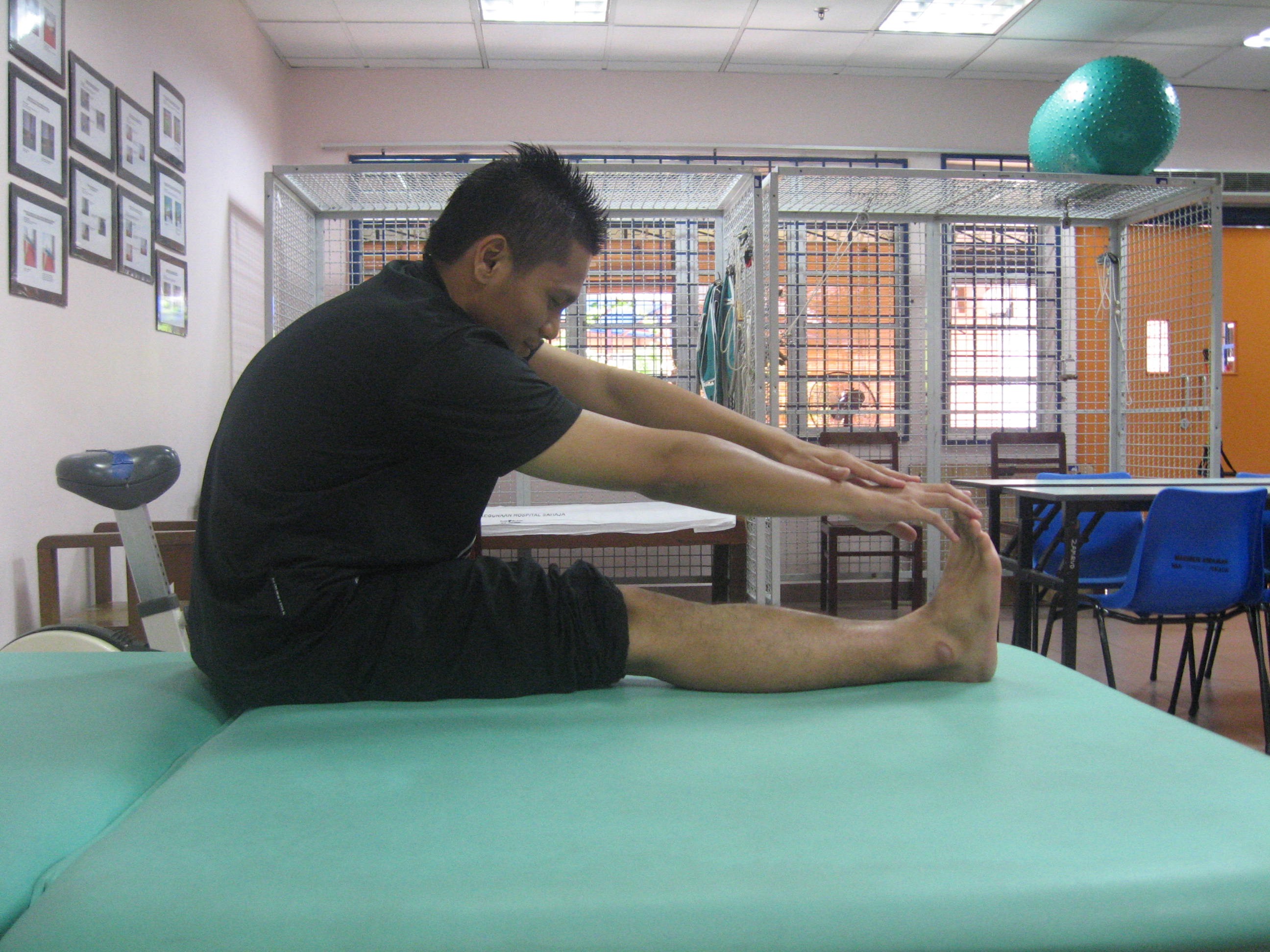
- Stretching exercise
 |
 |
|
| Self-stretching for hamstring Position : Long sitting Instruction : Straighten knee & lift up ankle, 30 secs hold(8-10 repititions |
Self-stretching for calf Position : Standing against wall Instruction : Straighten knee & foot fully placed on the floor, 30 secs hold (8-10 repititions) |
|
Source: Unit Fisioterapi Hospital Melaka
- Strengthening exercise
- Isometric contraction
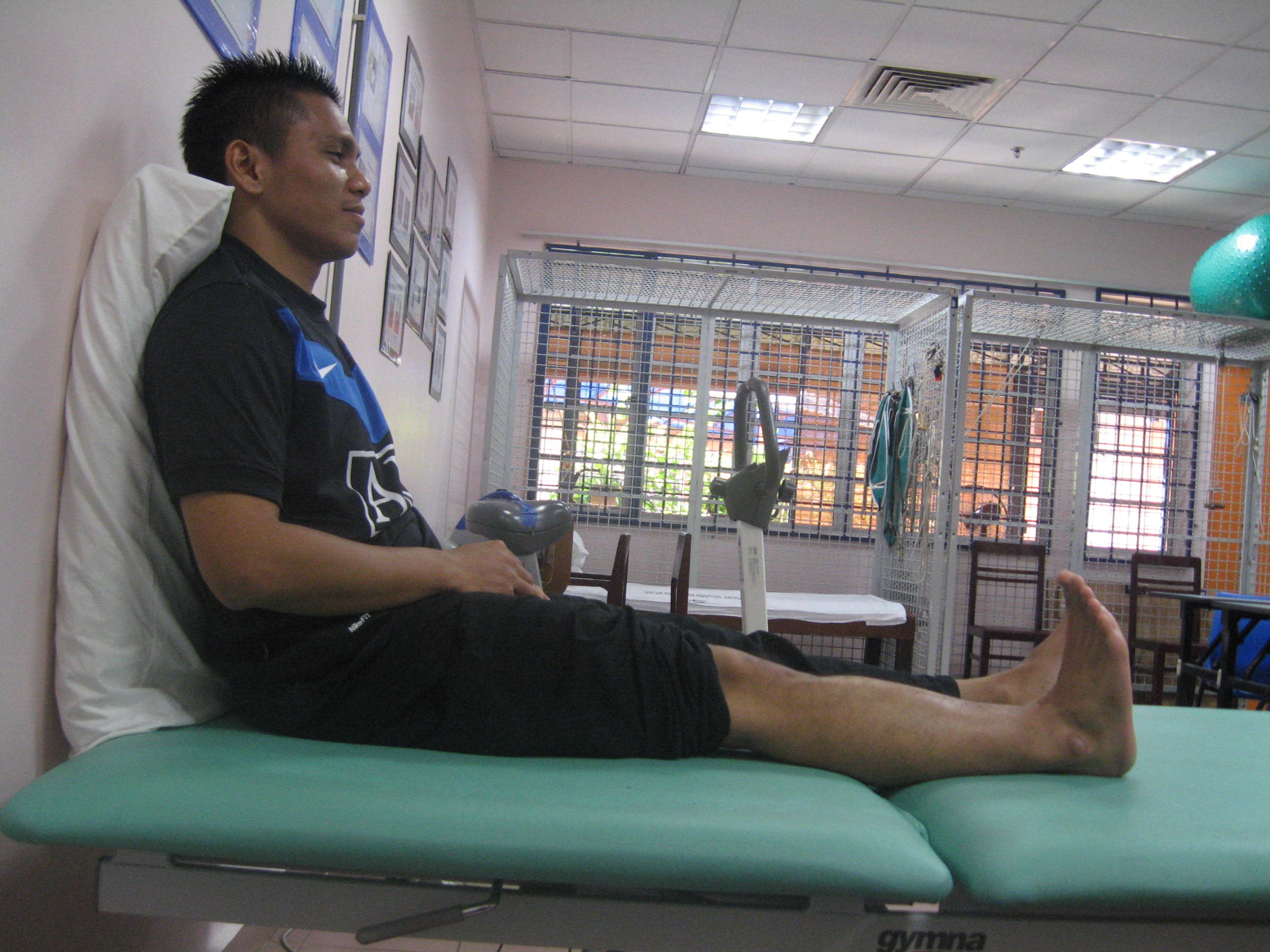 |
| Quadriceps Isometric contraction Position : Long sitting or standing Instruction : Straighten knee & pointing ankle towards knee 30 secs hold(8-10 repititions/2-3 sets) |
Source: Unit Fisioterapi Hospital Melaka
- Slow resistance exercise (improve strength)
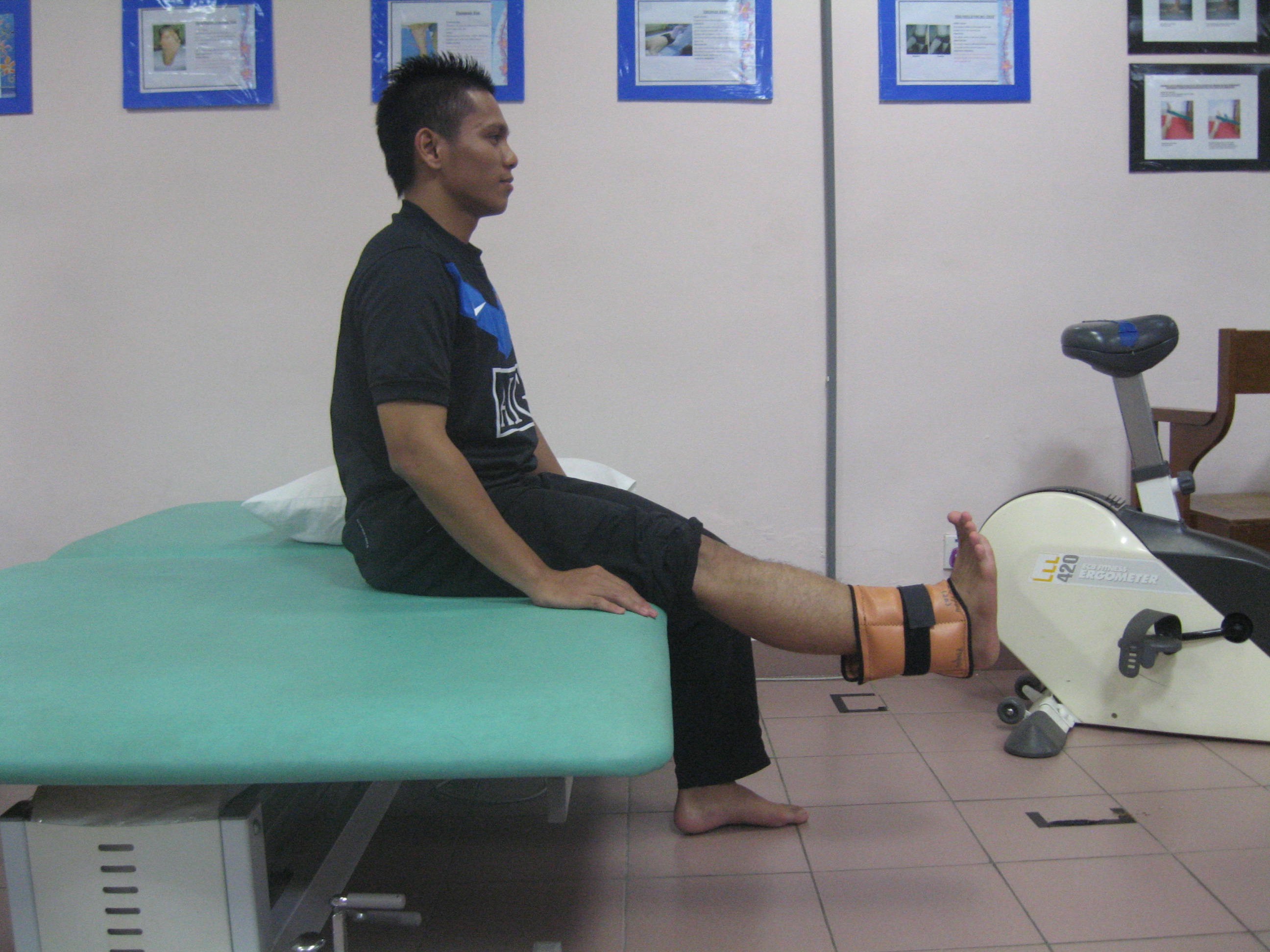 |
| Quadriceps Isotonic Strengthening Position : Upright sitting Instruction : Straighten knee & pointing ankle towards knee 15secs hold (8-10 repititions/2-3 sets) |
Source: Unit Fisioterapi Hospital Melaka
- Functional strengthening
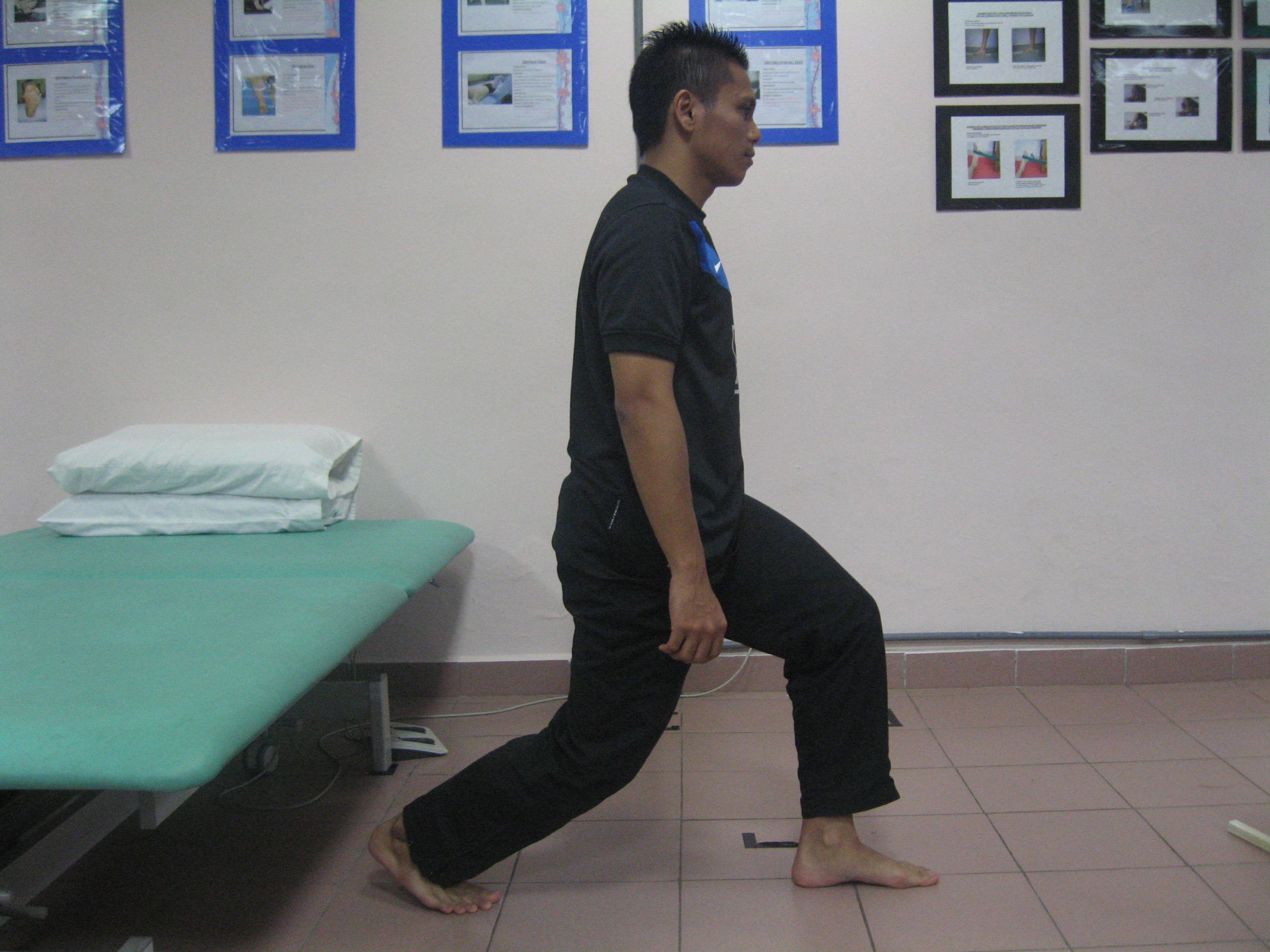 |
| Lunges Position : Affected leg in front Instruction : Bending hip & knee & maintain knee behind vertical imaginary line from the toe (8-10 repititions/ 2-3 sets) |
Source: Unit Fisioterapi Hospital Melaka
- Proprioceptive training
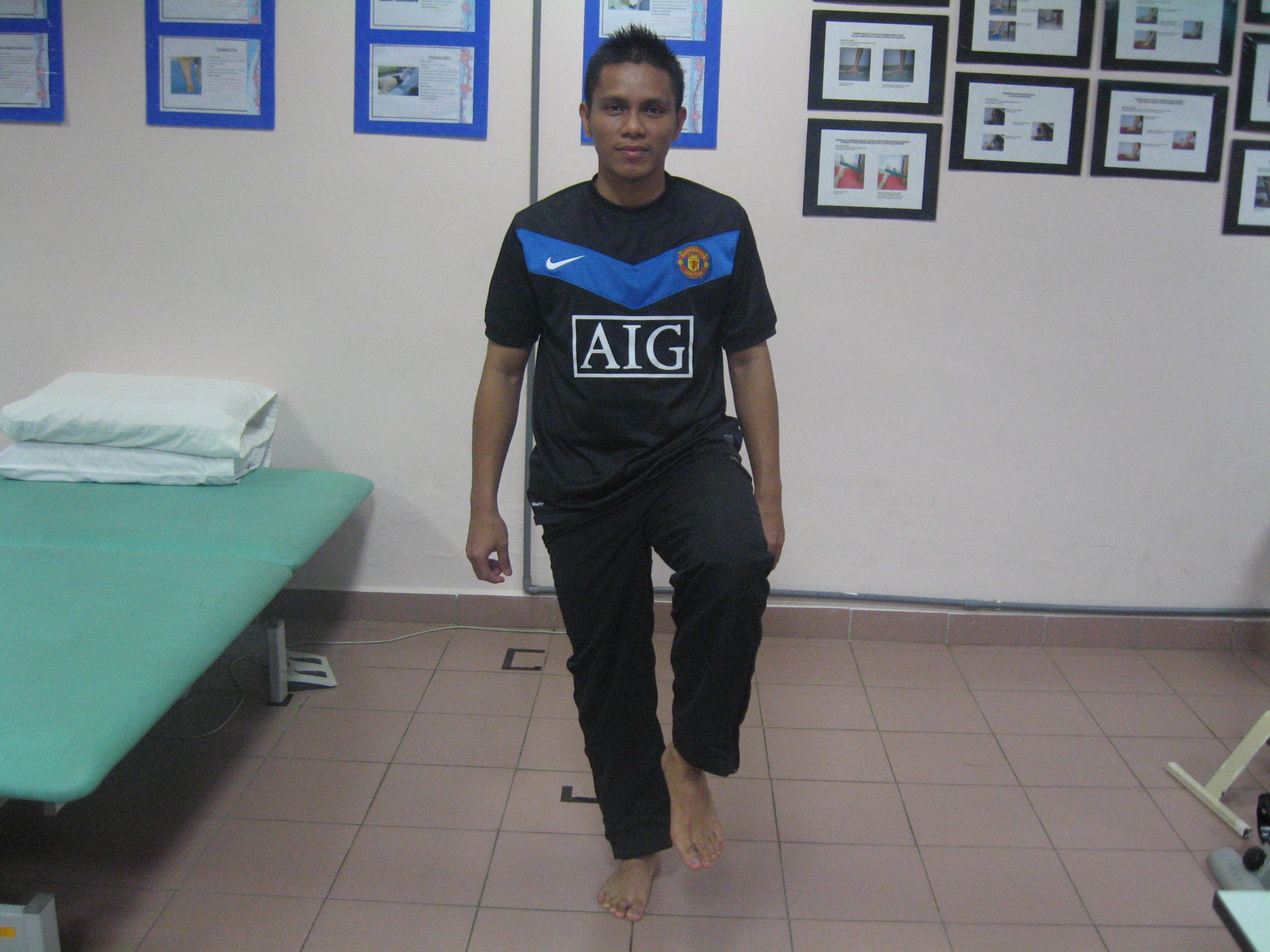 |
| Single-leg standing (eyes open àeyes closed) Position : Sitting on affected leg Instruction : Keep the affected leg straight 30 secs hold (3 repititions) |
Source: Unit Fisioterapi Hospital Melaka
- Education
Regular pain monitoring will help guide and progress the exercise programme and should be maintained after return to sport.
Exercise is the superior of Jumper’s Knee management and well-rounded rehabilitation programme involving kinetic chain exercises, education in proper landing technique and management of load and return to sports (Cook JL, Purdam CR., 2014)
References
- Zwerver J, Bredeweg SW, van den Akker-Scheek I. Prevalence of Jumper’s knee among non elite athletes from different sports: a cross-sectional survey. Am J Sports Med. 2011;39:1984–1988. 3
- Kannus P, Natri A. Etiology and pathophysiology of tendon ruptures in sports. Scand J Med Sci Sports. 1997;7:107–112. 5
- Visnes H, Bahr R. Training volume and body composition as risk factors for developing jumper’s knee among young elite volleyball players. Scand J Med Sci Sports. 2013;23:607–613. 16
- Crossley KM, Thancanamootoo K, Metcalf BR, Cook JL, Purdam CR, Warden SJ. Clinical features of patellar tendinopathy and their implications for rehabilitation. J Orthop Res. 2007;25:1164–1175. 18
- Malliaras P, Cook JL, Kent P. Reduced ankle dorsiflexion range may increase the risk of patellar tendon injury among volleyball players. J Sci Med Sport. 2006;9:304– 309. 23
- Malliaras P, Cook JL, Kent PM. Anthropometric risk factors for patellar tendon injury among volleyball players. Br J Sports Med. 2007;41:259–263. 26
- Stasinopoulos D, Stasinopoulos I. Comparison of effects of exercise programme, pulsed ultrasound and transverse friction in the treatment of chronic patellar tendinopathy. Clin Rehabil. 2004;18:347–352. 50
- Pedrelli A, Stecco C, Day JA. Treating patellar tendinopathy with Fascial Manipulation. J Bodyw Mov Ther. 2009;13:73–80. 51
- Cook JL, Purdam CR. The challenge of managing tendinopathy in competing athletes. Br J Sports Med. 2014;48:506–509. 38
Source image
- (2015) Unit Fisioterapi Hospital Melaka. Retrieved October 29 2015
| Last Reviewed | : | 23 August 2019 |
| Writer | : | Mohd Naqiuddin bin Johar |
| Accreditor | : | Se To Phui Lin |
| Reviewer | : | Halimah bt. Hashim |







