What is Nephrotic Syndrome?
Nephrotic syndrome (NS) is a clinical syndrome characterized by :
- swelling of the face, limbs or body (oedema)
- leakage of protein in the urine (proteinuria) of more than 3 g/day
- low serum protein/albumin (hypoalbuminemia)
- high cholesterol level (hypercholesterolemia)
How common is Nephrotic Syndrome?
- It can occur at any age
- Is more prevalent in children
- In children, it occurs commonly between ages 1 1/2 and 4 years and is more common in young males
- The sex distribution is equal in older patients
What are symptoms and signs of Nephrotic Syndrome?
The possible symptoms and signs are as follows :
- Oedema
- Oliguria (Reduces amount of urine)
- Passing frothy and foul smelling urine
- Hypertension (Occasional)
- Poor general well being
- Haematuria (rare)
What is oedema?
Oedema is usually an early manifestation of NS and occurs in approximately 95% – 99% of cases. It is the natural consequence of hypoalbuminemia. Oedema in the early phase usually starts around the eyes (periorbital oedema) and is often worse in the face upon rising in the morning.
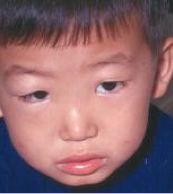
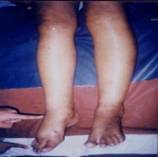
It gradually progresses to involve the limbs and will produce pittingon pressure. The swelling of the lower extremities becomes more predominant in the later part of the day (oedema is dependant in nature).
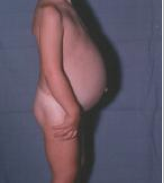
In later stages, it may cause abdominal distension (ascites) due to accumulation of fluid in abdominal cavity.
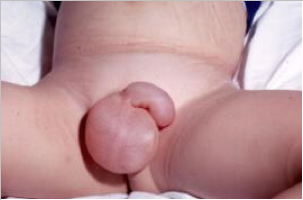
There may also be scrotal or labial swelling.
As the disease progress, the edema becomes more generalized (anasarca). There may be difficulty in breathing due to fluid accumulation around the lungs (pleural effusion) Sometimes, oedema is so subtle in onset that it is attributed to weight gain. Occasionally clear fluid may ooze from the surface of the skin.
What is oliguria?
Oliguria refers to the reduction in the quantity (volume) of total urine output in a day. The normal urine output is about 1.5 liters/day.
What is hypertension?
Hypertension denotes a raised blood pressure. (link to Screening for Hypertension and Hypertension)

What is poor general well being?
- Feeling unwell or lethargic
- Loss of appetite (anorexia)
- Easy fatigability and irritability
What is haematuria?
Presence of blood in the urine – macroscopic (visible to the naked eye) or microscopic (visible only under the microscope). May occur in some forms of Nephrotic Syndrome.
What are the complications of Nephrotic syndrome?
- Thrombo-embolism
A patient with Nephrotic Syndrome may develop severe pain and swelling in one or both legs. This is due to clotting of blood in the blood vessels of the lower limbs.
- Susceptibility to infections
Common sources of infection are the peritoneum (peritonitis) and the urinary tract (urinary tract infection). Symptoms can vary from fever, abdominal pain, diarrhoea, painful or burning urination.
- Increase in bowel movements (diarrhoea)
Usually due to gut wall oedema. May indicate peritonitis if accompanied by fever.
What to do if you suspect you have Nephrotic Syndrome?
Seek medical advice for confirmation and treatment.
What investigations are required for the diagnosis of Nephrotic Syndrome?
- Urinalysis
- Blood analysis
- Kidney ultrasound and biopsy (if indicated only)
Urinalysis
|
 |
|
 |
- Urinalysis may show the presence of blood in the urine.
Blood analysis
- Serum albumin of less than 25 g/L.
- Hypercholesterolaemia is a common finding
- Blood urea nitrogen and creatinine, level arean indicator of kidney damage. High levels of these metabolic products indicate accompanying impairment of kidney function.
Kidney ultrasound and biopsy
Routine imaging studies are not indicated in Nephrotic Syndrome. However, it is usually done prior to performing a renal biopsy to ensure the presence of two kidneys.
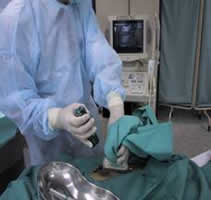
In some cases, the doctor may want to examine a small piece of the patient’s kidney under a microscope to determine the underlying cause and extent of disease. The procedure of getting a tiny sample of tissue from the kidney is called a biopsy. This procedure is done under aseptic technique. A local anaesthetic agent is used to provide pain relief.
 |
|
 |
|
What are the complications of a renal biopsy?
- Pain at the site of biopsy
- Bleeding – the most common complication. However, it is most often minor
- Passing blood in the urine – can occur, usually transient
- Haematoma – collection of blood around the kidney. Commonly small and asymptomatic
What is the treatment of Nephrotic Syndrome?
- Differs between adult and children
- Would depend on the cause of the Nephrotic Syndrome
- However, there are some non-specific therapies which include :
- Diet
A normal protein diet with adequate calories is recommended.
- Fluid and salt restriction
Fluid should be restricted according to urine output. (Total fluid intake advised is volume of previous day urine output + 500mls for losses due to sweating, bowel motions, etc). Salt intake should be reduced to prevent fluid and salt retention. No added salt to food is recommended.
- Diuretic medication
Diuretics are generally advocated to increase urine output. May need to be administered intravenously.
- Anti-hypertensives
Choice of an agent would be one that can offer good blood pressure and simultaneously decrease the severity of proteinuria.
Specific Treatment for Nephrotic Syndrome in CHILDREN
In children, about 80% of children aged 1 to 12 years old have minimal change disease. Of these, more than 90% respond to corticosteroid therapy and therefore a renal biopsy is not warranted. Corticosteroid was found to be effective in inducing remission of NS and has been the first line therapy. A child with NS who fails to respond to an initial 4 week treatment with corticosteroid should be referred to a nephrologist for a renal biopsy.
Further Information: Refer to Consensus Statement of Management of Idiopathic Nephrotic Syndrome in Childhood 1999 which is available on the website www.acadmed.org.my under clinical practice guidelines.
Specific Treatment for Nephrotic Syndrome in ADULTS
Specific treatment offered will depend on the results of the biopsy.
Data from the Report of the Malaysian Registry of Renal Biopsy 2008 indicates the commonest causes of Nephrotic Syndrome are :
- Minimal Change Disease – 27%
- Lupus Nephritis – 24%
- FSGS (Focal Segmental Glomerulosclerosis) – 23%
- Membranous Nephropathy – 6%
Specific management of complications of Nephrotic Syndrome
- Infection
Patients with NS are prone to infections especially peritonitis and cellulitis. Appropriate antibiotics are required.
- Kidney Failure.
This is a known complication. It may be due to dehydration, overdiuresis or swelling of the kidney tissue. However, this form of kidney failure is generally reversible.
- Thrombosis
This complication can be life threatening and requires anticoagulation therapy. Sometimes prophylactic anticoagulation is required to prevent this complication.
| Last reviewed | : | 26 April 2012 |
| Writer | : | Dr. Anita Bhajan Manocha |
| Reviewer | : | Dr. Sunita a/p Bavanandan |







