Definition
Melasma is a brown, tan or blue-gray discoloration on the face. It is most common in women 20 to 50 years of age. Men can also be affected.
Cause
Melasma is thought to be caused partly by sun exposure, genetic predisposition, and hormonal changes due to birth control pills, pregnancy and medications that can make the skin more prone to pigmentation after exposure to ultraviolet (UV) light. Melasma in pregnancy, is an often referred to as chloasma or “the mask of pregnancy.” Pregnant women have increased level of estrogen, progesterone, and melanocyte-stimulating hormone (MSH) during the second and third trimester of pregnancy. Melanocytes are skin cells that deposit pigments in the skin and produce pigmentation. In addition, any products or treatments that irritate the skin may cause an increase in melanin production and accelerate melasma appearance.
Clinical presentations
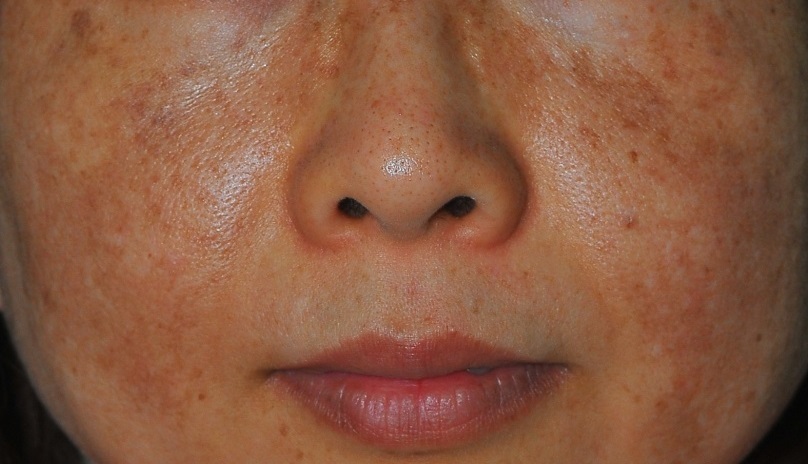
Melasma can present in three sites; central face, cheekbone, and jawline (Photo 1). Therefore at the center of the face, it typically appears on the upper cheeks (Photo 2), upper lip, forehead and chin. The malar pattern will involve the cheekbone area and the mandibular pattern will affect the jaw area.
 |
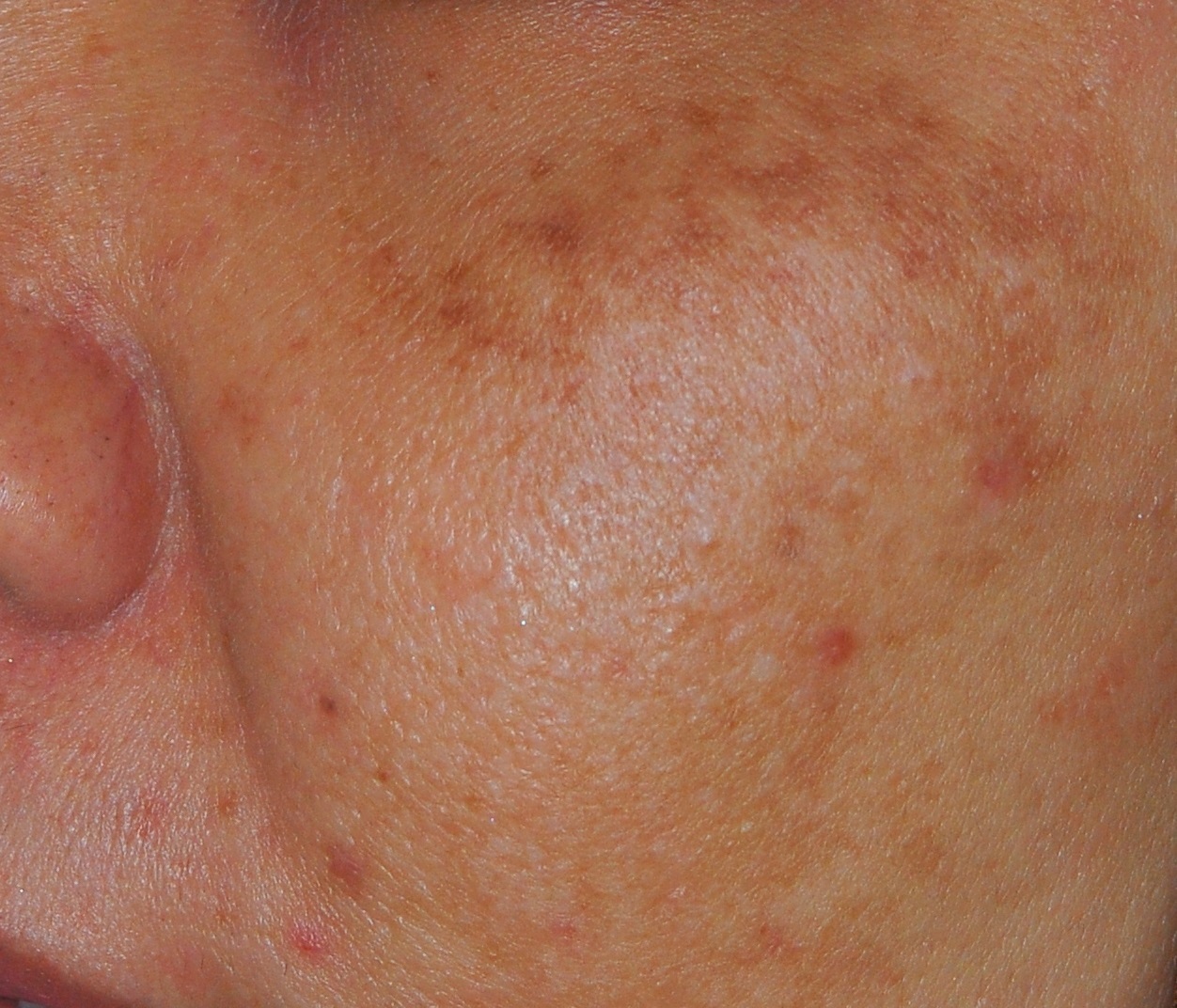 |
| Photo 1: Melasma usually occur on both sides of the face | Photo 2: Brownish pigmentation on upper cheek |
Treatment
The response to treatment for melasma depends on the types of melasma. The more superficial type or epidermal type responds better to treatment as compared to the dermal type because the pigment is closer to the skin surface.
Treatment requires regular sunscreen application and applying bleaching medications such as hydroquinone. The 2 most commonly used creams contain 2% hydroquinone (HQ) and doctor’s prescription-strength 4% hydroquinone. Sunscreen should be applied over the hydroquinone cream every morning. Certain sunscreens also contain 4% hydroquinone.
Any combinations or specially formulated creams with hydroquinone, a phenolic hypopigmenting agent, azelaic acid, and retinoic acid (tretinoin), nonphenolic bleaching agents, and/or kojic acid may be prescribed. In severe cases, a higher concentration of HQ or combining HQ with other ingredients such as tretinoin, corticosteroids, or glycolic acid may be effective in lightening the skin.
Possible side effects of melasma treatment include temporary skin irritation. The use of HQ in very high concentrations for prolonged periods (usually several months to years) may cause ochronosis. This is a permanent skin discoloration that can occur from the use of hydroquinone concentrations above 4%. Despite the potential side effects, HQ remains the most widely used and most successful treatment. HQ should be discontinued at the first sign of ochronosis.
Other treatments include Lactic acid lotions 12%, Glycolic acid 10-20% creams and Glycolic acid peels 10-70%. Chemical peels (chemical exfoliation) of high concentration can only be applied by a trained personnel as a clinic based treatment. It may be useful for some cases of melasma. The type of chemical peel used should be tailored to each individual and selected by the physician.
Azelaic acid is effective in treatment of melasma, although the overall results are significantly less impressive than 4% hydroquinone. Possible minor side effects include itching (pruritus), redness (erythema), scaling (dry patches), and a temporary burning sensation that tends to improve after 14 to 30 days of use.
With tretinoin cream, melasma may respond slower with no hydroquinone combination. Tretinoin cream can cause mild localized side effects such as peeling of the skin, dry skin, and irritation.
There are combined doctors’ prescription creams containing fluocinolone acetonide 0.01%, hydroquinone 4%, and tretinoin 0.05%. It is used to treat melasma and other skin discoloration. Results may be usually seen at about six to eight weeks later. It should not be used for prolonged periods exceeding eight weeks without your doctor’s recommendation. It should not be used by pregnant or breastfeeding women unless specifically instructed by your physician.
Other combined creams include the Kligman formula, a triple cream which include a retinoid, a hydroquinone, and a topical steroid (for example, fluocinolone acetonide 0.01%, hydroquinone 8%, and tretinoin 0.1%). These triple combination cream may be compounded in different strengths according to a physician’s prescription. Triple creams are highly effective for melasma.
Multiple treatments in combination with sunscreen and other creams yield good results. However there is no guarantee that melasma can be improved with these creams. It is very important to be aware if the treatments are too harsh or abrasive, melasma can be induced or worsen. These are cosmetic procedures that will not be covered by medical insurance providers.
To prevent treatment failure, sun exposure must be minimized. Many melasma creams need to be discontinued in pregnancy and breastfeeding because of possible risks to the developing fetus and newborn. These people may consider cosmetics to temporarily conceal the skin discoloration.
The role of laser in melasma treatment
Lasers may be used in melasma but it is not the primary choice of treatment as the result may not achieve certain expectation. Lasers may actually worsen certain types of melasma and should be used with caution. Multiple treatments may be necessary to see results.
Recommended sun protection factor SPF
A daily sun protection which contains physical blockers, such as zinc oxide and titanium dioxide, is recommended to block UV rays. The commonly available chemical blockers have a SPF of 30. Chemical blockers may not fully block both UV-A and UV-B as effectively as zinc or titanium.
Prevention
To prevent melasma formation, sun avoidance and sun protection with hats and sunscreen are required. Melasma may clear spontaneously without treatment but it is advisable to use sunscreen and avoid sun exposure. Melasma may also disappear following delivery or if birth control pills and hormone therapy are discontinued.
Reference
- Freedberg, Irwin M., et al. Fitzpatrick’s Dermatology in General Medicine. 4th ed. Vol. 1. New York: McGraw-Hill, 1993.
- Rashmi Sarkar, Shikha Chugh, Vijay K Garg. Newer and upcoming therapies for melasma. Indian J Dermatol Venereol. 2012; 78(4): 417-428.
- Kabir Sardana, Vijay K Garg Lasers are not Effective for Melasma in Darkly Pigmented Skin. Journal of Cutan and Aesthet Surg. 2014; 7 (1): 57-60.
- Pooja Arora, Rashmi Sarkar, Vijay K Garg, Latika Arya Lasers for Treatment of Melasma and Post-inflammatory Hyperpigmentation Journal of Cutaneous and Aesthetic Surgery. 2012; 5(2): 93-103.
- Tania Ferreira Cestari, Lia Pinheiro Dantas, Juliana Catucci Boza. Acquired hyperpigmentations. An Bras Dermatol. 2014; 89(1):11-25.
| Last Reviewed | : | 23 August 2019 |
| Writer/Translator | : | Datin Dr. Asmah bt. Johar |
| Accreditor | : | Datuk Dr. Roshidah bt. Baba |
| Reviewer | : | Dr. Nazatul Shima bt. Abd Rahim |







