Introduction
A hormone is a chemical released by a cell, gland or an organ in the body that affects cells in other parts of the body. The terms “menstruation” and “menses” are derived from mensis in Latin, which means month. In humans, the menstrual cycle occurs monthly, with an average of 28 days per cycle.
The length of menstrual cycles is counted from the first day of menstrual bleeding until the first day of next cycle. The occurrence of regular menstrual cycles depends on the complex interactions of hormones between the pituitary, ovaries and uterus. Ovarian follicles are the basic units of female reproductive system. A follicle is composed of aggregations of cells in the ovary. It contains an immature ovum (egg).
The changes in the cycle are essential for the production of eggs and preparation of the uterus for pregnancy. Therefore, the menstrual cycle can be manipulated using hormonal contraception to prevent reproduction. The menstrual cycle occurs only in fertile female humans and other female primates.
Hormones in Menstrual Cycle
The pituitary gland in the brain produces the Follicle Stimulating Hormone (FSH) and Luteinizing Hormone (LH) during the menstrual cycle. The types of hormones involved in the menstrual cycle and their functions are as shown in the table below:
| Hormones | Function |
| FSH | Stimulates one or few follicles in the ovary to develop into an egg.
|
| LH | Causes the mature egg to be released from the ovary in a process known as ovulation. LH also stimulates the corpus luteum (empty follicle of the mature egg) to produce progesterone.
|
| Estrogen/Estradiol | The ovaries produce estrogen to initiate the repair of the uterus lining of the shed in the last menstruation
|
| Progesterone | Causes the lining of the uterus to thicken and ready for the implantation of a fertilized egg
|
Hormonal Changes During Menstrual Cycle
The menstrual cycle is divided into three phases:
- follicular or proliferative phase
- ovulatory phase
- luteal or secretory phase
During the follicular phase, the FSH rises and stimulates a few ovarian follicles to grow. One of the follicles becomes dominant and continues to mature. At the same time, the ovary produces estrogen and causes the FSH to fall and LH to rise.
The LH rises to its peak at 34 to 36 hours before ovulation. The mature follicle ruptures and releases the egg from the ovary. The egg is then swept into the fallopian tube. The mature egg is either fertilized by a spermatozoon or degenerates if it is not fertilized after about a day.
After ovulation, the ruptured follicle transforms into corpus luteum. Corpus luteum produces progesterone and estrogen. Both of these hormones will cause the LH and FSH concentrations to fall off.
The corpus luteum degenerates towards the end of luteal phase. Subsequently, the levels of estrogen and progesterone decrease. The hormonal drop causes the uterus to shed its lining and unfertilised egg in a process termed menstruation (also called menstrual bleeding, menses, or period).
Subsequently, the pituitary gland is stimulated to produce FSH and a new cycle begins.
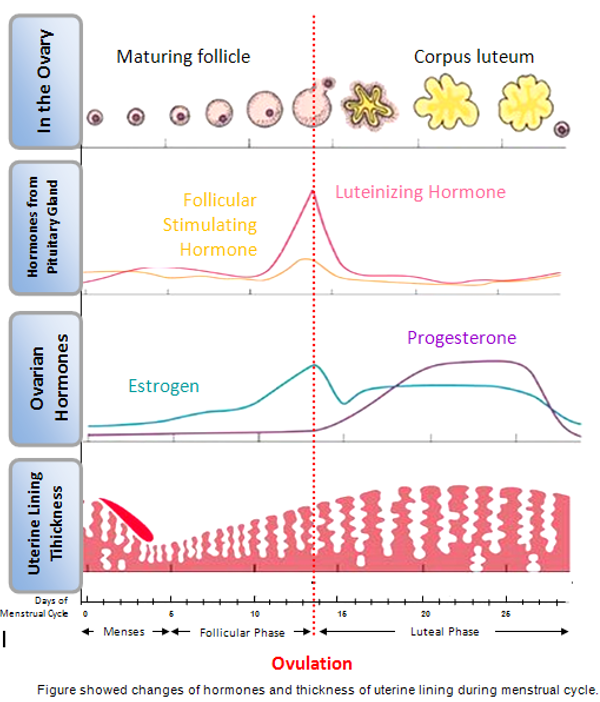
The figure below shows changes of hormones and thickness of uterine wall during menstrual cycle
 Preparation Prior to Taking Sample
Preparation Prior to Taking Sample
Testing of FSH, LH, progesterone and estrogen levels can help to find the cause of infertility. These tests are used subsequently to monitor the effect of infertility treatment, if required. The tests also help to diagnose problems with the pituitary gland and some types of cancer.
The testing is carried out using blood sample. More than one blood sample can be taken each day for several days in a row to identify problems in menstrual cycle.
These tests may be affected by certain medicines (including birth control pills). Recent exposure to radioisotopes (e.g. nuclear medicine scan) with a week can also affect the test results.
Information on the menstrual cycle such as date of first day of last menstrual period and pregnancy should be noted before initiating these tests.
Test Methods
The most common testing method for FSH and LH is two-site chemiluminometric (sandwich) immunoassay.
The estradiol and progesterone levels are measured with immunoassay using competitive chemiluminescent technology.
Reference Range – Test Results
The reference ranges differ depending on a person’s age, gender, menstrual cycle phase and pregnancy.
| TEST | FEMALE | MALE | |
| FSH | Before puberty | 0 – 4.0 IU/L | 0 – 5.0 IU/L |
| During puberty | 0.3 – 10.0 IU/L | 0.3 – 10.0 IU/L | |
| Adult | 4.7 – 21.5 IU/L (menstruating) | 1.5 – 12.4 IU/L | |
| 25.8 – 134.8 IU/L (post-menopausal) | |||
| LH | Follicular phase | 1.9 – 12.5 IU/L | Age 20 – 70:
0.7 – 7.9 IU/L |
| Peak of menstrual cycle | 8.7 – 76.3 IU/L | > 70 years:
3.1 – 34 IU/L |
|
| Luteal phase | 0.5 – 16.9 IU/L | ||
| Post menopausal | 15.9 – 54.0 IU/L | ||
| Estradiol | 20 – 750 pg/mL
(menstruating) |
14 – 55 pg/mL | |
| < 35 pg/mL
(post-menopausal) |
|||
| Progesterone | Menstrual Cycle
Day 1 – 14 Day 15 – 28 |
< 1 ng/mL or 0.5 – 2.3 nmol/L
2 – 25 ng/mL or 6.4 – 79.5 nmol/L |
< 1 ng/mL or
< 3.2 nmol/L |
| Pregnancy
First trimester Second trimester Third trimester |
10 – 44 ng/mL or 32.6 – 140 nmol/L 19.5 – 82.5 ng/mL or 62 – 262 nmol/L 65 – 290 ng/mL or 206.7 – 728 nmol/L |
||
| Post-menopausal | <1.0 ng/mL or
< 2 nmol/L |
References
- Silverthorn, Dee Unglaub (2013). Human Physiology: An Integrated Approach (6th). Glenview, IL: Pearson Education, Inc. pp. 850–890. ISBN0-321-75007-1.
- Klump KL, Keel PK, Racine SE, et al. (February 2013). “The interactive effects of estrogen and progesterone on changes in emotional eating across the menstrual cycle”. J Abnorm Psychol 122 (1): 131–7. doi:1037/a0029524. PMID22889242.
- Kaplan LA, Pesce AJ, Kazmierczak SC. Clinical Chemistry: Theory, Analysis, Correlation (4th) Mosby, Inc. pp. 851-857. ISBN 0-323-01716-9.
- http://labtestsonline.org/understanding/analytes/estrogen/tab/ask
- http://women.webmd.com/progesterone
| Last Reviewed | : | 31 January 2016 |
| Writer | : | Katheleen Ng Li Fong |
| Accreditor | : | Lau Kim Bee |







