What is denture related stomatitis?
Denture related stomatitis (DRS) is also known as denture sore mouth, denture stomatitis or candida-associated denture induced stomatitis. It is a common disorder affecting denture wearers. This condition is seen mostly among the elderly (as they are more likely to be using dentures), especially those living in nursing homes/facilities. The common presentation is that of inflammation and redness of the area covered by the denture base. Pain / Discomfort are usually not present till later stages of the condition.
How does it happen?
Although the majority of cases are associated with the fungal organism Candida albicans, there have been reports of denture related stomatitis being caused by bacterial organisms as well. As such, the cause of denture related stomatitis is best described as being multifactorial.
Several factors have been established as being risk-factors:
- Poor denture and oral hygiene
- Continual and night-time use of removable dental prostheses
- Poorly fitting dentures
- Underlying systemic problems such as diabetes mellitus
All the above mentioned factors increase the ability of opportunistic pathogens such as Candida albicans to colonize both the denture and the underlying mucosa. Poorly fitting dentures also cause mucosal trauma. Denture related stomatitis however is not caused by pure allergy to the denture material.
Denture related stomatitis has been classified depending on the severity of the condition. The following is the commonly used Newton’s classification system:
Type I: Pinpoint redness or localized simple inflammation
Type II: Diffuse redness confined to the mucosa contacting the denture.
Type III: Granular surface or inflammatory papillary hyperplasia of the palate
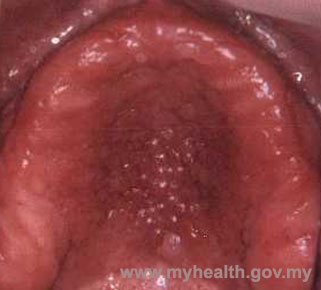
Type III Denture related stomatitis with a granular and papillary palate
Type I is thought to be the early or initial stages of denture related stomatitis whilst Type III is rare and is a manifestation of the response to chronic inflammatory stimulation secondary to microbial colonization as well as an element of trauma from an ill-fitting dentures.
How does the dentist diagnose this condition?
A thorough clinical examination of the mouth and dentures is usually sufficient to achieve a diagnosis of denture related stomatitis. The classical clinical presentation of erythema and oedema of the mucosa covered by the denture base but not extending beyond is a diagnostic finding. At times, a smear of the mucosa is performed and stained with potassium hydroxide (KOH) or periodic acid-Schiff to detect the presence of fungal organisms.
How is it treated?
Management of this condition can be subdivided into the following categories and usually involves a combined approach:
- Oral hygiene
The mouth must be kept as clean as possible and one should rinse after meals.
-
Denture hygiene & adjustment of existing dentures
The existing dentures should be cleaned and any necessary adjustments should be performed to minimise trauma to the underlying tissue as well as to eradicate the microbial component on the dentures. The dentures should be left out of the mouth as much as possible and overnight usage (whilst sleeping) should be stopped. Many times, early stages of denture stomatitis will resolve completely if the dentures are not worn at night for about 2 – 3 weeks. Get more information on caring for dentures as well as preventing denture stomatitis.
-
Medication
If conservative measures of hygiene and cleaning have been unhelpful, the clinician may decide to prescribe some topical medication. The most commonly used medications would be antifungal ointments/lozenges/suspensions as well as antibacterial mouthrinses. Although antimicrobial treatment can remove/reduce microbial contamination and provide temporary resolution of the denture related stomatitis, without proper denture & oral hygiene, the stomatitis will recur when antimicrobial therapy is discontinued.
-
Surgery
At times, especially for Type III denture related stomatitis, minor oral surgery has to be performed to remove any excess tissue to facilitate construction of new dentures. Besides that, for Type III denture related stomatitis, due to the presence of papillary and granular tissue, a biopsy may be performed to rule out other disease processes that may present in a similar manner.
-
Construction of new, better fitting dentures
After the mucosa has achieved adequate healing and the patient has shown better oral as well as denture hygiene, construction of better fitting dentures will usually be performed.
What are the possible complications?
If left untreated, denture related stomatitis can cause pain/discomfort in the mouth and may lead to poorly fitting dentures in the future.
References
- Newton AV. Denture sore mouth as possible etiology. Brit Dental J. 1962;112:357-60.
- Wilson J. The aetiology, diagnosis and management of denture stomatitis. Br Dent J. Oct 24 1998;185(8):380-4
- Naik AV, Pai RC. A study of factors contributing to denture stomatitis in a north Indian community. Int J Dent. 2011
- Scully, Crispian (2008). Oral and maxillofacial medicine : the basis of diagnosis and treatment (2nd ed. ed.). Edinburgh: Churchill Livingstone. pp. 201–203.
| Last Reviewed | : | 24 January 2014 |
| Writer | : | Dr. Hans Prakash a/l Sathasivam |
| Accreditor | : | Dr. Abdul Rahim bin Ahmad |







