Introduction
The morphology of sperm cells is the end result of a highly complex process of cellular modifications occurring during spermiogenesis. In humans, it leads to widely heterogenous morphological pattern, with many cellular abnormalities which may be associated with sperm dysfunction. The morphological assessment of human spermatozoa which includes the evaluation of the percentage of morphologically normal sperm and the determination of the incidence of various morphological abnormalities has always been part if semen analysis in couples consulting for infertility.
Computer Aided Sperm Analysis (CASA)
Computer aided semen analysis (CASA); also known as sperm quality analyzer, computer assisted sperm motility analysis, and a microcomputer-photographic method for evaluation; has been used for many years to provide an objective measure of semen characteristics including assessment of motility, concentration and morphology. However, the focus of this article is going to be on the assessment of image analysis to indicate the normal sperm morphology of an ejaculate.
The regular set up consists of a microscope, a video camera and morphology software. The computer frame grabber receives images from the video camera for analysis by the morphology software. These measurements are used to assign the sperm to different classifications; normal, subnormal, or abnormal.
Morphological assessment of sperm
Sperm morphology was assessed in the initial semen analysis using the Kruger-Tygerberg Strict Criteria as outlined by the World Health Organization. Using this criterion, any subnormally (or borderline forms) classified sperm cells are going to be indicated as abnormal.
In assessing the sperm morphology, these steps are involved:
- 5 – 10 µL of semen depending on the total count was placed on a cleane slide and smeared
- If the sperm concentration is low (<2 × 10x6 per ml), samples will need to be concentrated by centrifugation (centrifugation may affect sperm morphology)
- Air-drying the smear for at least 1 hour or left on top of warmer for 10-15minutes.
- Staining using the Diff Quik staining protocol (or any other suitable staining method)
- Examination of the slide with bright field optics at ×1000 magnification with oil immersion
- Assessing approximately 200 spermatozoa and the value of normal sperm is calculated in percentage.
Normal-shaped sperm
A normal sperm has:
- A smooth, oval-shaped head that is 5-6 micrometers long and 2.5-3.5 micrometers wide (less than the size of a needle point)
- A well-defined cap (acrosome) that covers 40% to 70% of the sperm head
- No visible abnormality of midpiece, or tail
- No fluid droplets in the sperm head that are bigger than one half of the sperm head size
- No duplicate segments.
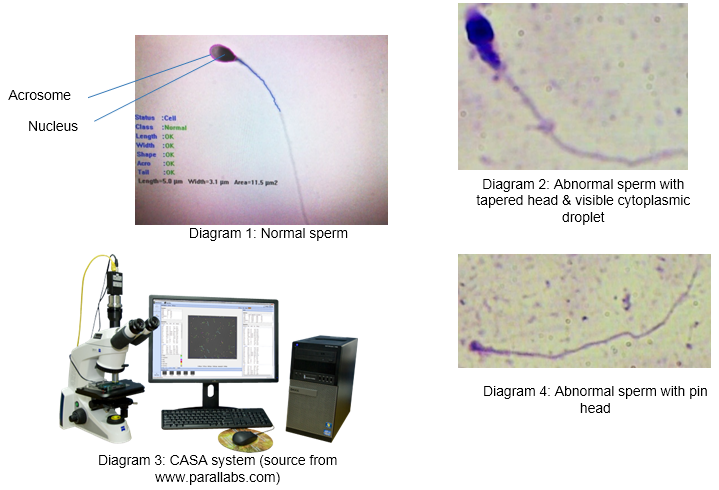
Examples of Sperm Morphology (Normal Vs Abnormal) & CASA System
Below are some of the sperm abnormalities observed in an ejaculate sample:
Advantages and disadvantages of assessing morphology using casa system:
|
Advantages |
Disadvantages |
|
|
Normal semen parameter (WHO 2010)
|
Parameter |
Value |
| Volume (ml) |
1.5 |
| Total sperm number (106 per ejaculate) |
39×106 |
| Sperm Concentration (106 per ml) |
15×106 |
| Total motility |
40% |
| Progessive motility |
32% |
| Vitality |
58% |
| Sperm morphology |
4% |
| pH |
7.2-7.8 |
Outcome
A study has reported significant relationships between automated morphology assessment results and fertility endpoints. Kruger, T.F. and Coetzee, K. (1999) found that the outcomes to be significant predictors of both fertilization rates in vitro and pregnancy.
More studies of fertility outcomes in large populations are required to refine the application of CASA to measuring sperm morphology. Automated systems may have a role in providing data for quality control systems, but more research is needed to demonstrate their benefit for clinics
References
- Auger, J., Eustache, F., Andersen, A. G., Irvine, D. S., Jorgensen, N., and Skakkebaek, N. E. et al. (2001). Sperm Morphological defects Related to Environment, Lifestyle and Medical History of 1001 male Partners of Pregnant Women from Four European Cities. Human Reproduction. 16. 2710-2717.
- Keegan, B. R. and Barton, S. (2007). Isolated teratozoospermia does not affect in vitro fertilization outcome and is not an indication for intracytoplasmic sperm injection. Fertility & Sterility (Vol. 88). 1583-1588.
- Kruger, T. F and Coetzee, K. (1999). The Role of Sperm Morphology in Assisted Reproduction. Human Reproduction Update (Vol. 5). 172 – 178.
- Nallella, K.P., Sharma, R.K., Aziz, N. and Agarwal, A. (2006). Significance of Characteristics in the Evaluation of Male Infertility. Fertility and Sterility. 85. 629-633.
- Ng, K.K., Donat, R., Lalak, A., Chan, L., Di Pierro, I. and Handelsman, D.J. (2004). Sperm Outpput of Older Men. Human Reproduction. 19. 1811-1815.
- O’ Connell, M., McClure, N. and Lewis, S.E.M. (2002). The Effects of Cryopreservation on Sperm Morphology, Motility And Mitochondrial Function. Human Reproduction. 17. 704-709.
- Thurston, L. M., Watson, P. F., Mileham, A.J. and Holt, W. V. (2001). Morphologically Distinct Sperm Subpopulations Defined by Fourier Shape Descriptors in Fresh Ejaculates Correlate with Variation in Boar Semen Quality Following Cryopreservation. Journal of Andrology (Vol. 22). 382-394.
| Last Reviewed | : | 14 April 2016 |
| Writer | : | Tajul Ariffin bin Isa |
| Accreditor | : | Krishnan a/l Kanniah |